Fetal Health Center
Finding out that your baby's health is at risk can be overwhelming. When expecting moms and babies need special care, Children’s Mercy is ready with the region’s most comprehensive and advanced care for select high-risk pregnancies before, during and after delivery.
Diagnosis and testing for fetal conditions
Each year, nearly 400 families like yours visit the Perinatal Clinic at the Elizabeth J. Ferrell Fetal Health Center for a consultation. Here, you'll have access to advanced diagnostic services like amniocentesis, fetal echocardiograms, and diagnostic ultrasound to help your health-care providers understand your baby’s condition. Our maternal-fetal medicine specialists coordinate with your obstetrician or primary-care provider to balance the needs of both you and your baby.
We treat thousands of babies with complex in-utero conditions each year. Parents often ask if we've seen a baby with a condition similar to theirs — the answer is yes. We see babies who have heart, gastrointestinal, lung, and other conditions that require immediate attention.
Every expert your child needs - including you
At Children’s Mercy, we build an integrated team which includes every fetal specialist who will be involved with your baby’s treatment.
As an active member of your baby's care team, you will sit around the table with every specialist your child may need at one time. We'll talk directly with you about your child's diagnosis and treatment options and discuss all your questions and concerns. Then, we will work together to create the best possible plan of care.
Your team may also include:
-
Genetic counselors
-
Social workers
-
Obstetrics and care coordinator nurses
-
Anesthesiologists
-
Sonographers and radiologists who specialize in prenatal imaging
Your world revolves around your baby – ours does too
There's no better place for a baby with complex medical needs than Children's Mercy. Our family-centered care approach helps you feel comfortable and informed during your time with us.
Some moms will deliver in our spacious and comfortable birthing suites – located right in the Fetal Health Center so their baby is always close by. Others will plan to deliver at another hospital, but come to Children's Mercy to meet with the doctors who will care for their baby after birth. Either way, you can work with the region’s best pediatric specialists right from the start.
Starting from your very first visit with us, you’ll have your own specially-trained care coordinator nurse who will get to know you and your family and stay with you every step of the way. He or she will help you with scheduling appointments, completing paperwork and communicating with all your doctors to make your experience as simple as possible. After your baby is born, you can continue to work with the doctors who already know your family's history in a friendly, child-centered environment.
See what you can expect when you visitWant a second opinion?
If you’ve recently received a diagnosis or would like a second opinion, experience matters. We're happy to share our expertise with you. Call (816) 855-1800 to make an appointment with our team.
Clinical Services
About one-third of families who come to the Fetal Health Center have a baby with a heart condition. As one of the top-ranking pediatric cardiology and heart surgery programs in the nation, Children's Mercy can help you through the process of getting an accurate diagnosis, understanding the condition, and finding the best possible course of treatment.
Innovative partnerships between Children’s Mercy researchers and physicians make it possible to treat or manage certain problems before a baby is even born with. The Children’s Mercy Fetal Treatment Team offer minimally-invasive therapies as well as advanced fetal surgery for complex conditions such as repair for spina bifida and twin-to-twin transfusion syndrome.
We want to meet the needs of postpartum mothers whose children are patients at Children's Mercy. Our postpartum services include resources for lactation, self-care for emotional health and healing from delivery. All our services are provided to help mothers of newborns take care of themselves.
Children’s Mercy provides safe and specialized transportation services for pregnant mothers at least 20 weeks gestation who need of immediate access to a higher level of care. Our team includes specialists for both mom and baby and is ready for dispatch 24 hours a day, seven days a week.
More than 1,000 babies have been delivered at the Fetal Health Center since the doors opened. Some of the first babies we delivered are now healthy, active grade-schoolers. For babies who need immediate care from their team of specialists or the region’s highest level neonatal intensive care unit (NICU), Special Care Delivery provides a meaningful birthing experience for you and immediate access to health experts for your baby.
Conditions
The team at the Fetal Health Center works with expectant mothers to diagnose, evaluate and treat all types of conditions before the baby is born. The list below details many—though not all—the conditions we commonly treat at the Fetal Health Center.
Clubfoot is a foot deformity where the foot and ankle did not develop normally in the womb.
Congenital diaphragmatic hernia (CDH) is a condition in which the diaphragm fails to close during prenatal development and the contents from the abdomen move into the chest.
We treat all types of cardiac conditions in the Fetal Cardiology Program. If your baby has a condition that requires continued care or surgery in the future, our top-ranked Heart Center team can help.
We treat a wide variety of congenital lung conditions found in infants, including congenital pulmonary airway malformation (CPAM) and congenital cystic adenomatoid malformation (CCAM).
Duodenal atresia is when the first part of the small intestine (the duodenum) does not completely develop in utero.
Encephalocele is a birth difference in which an opening in the skull allows a section of the brain and its coverings to bulge out into a sac.
Esophageal atresia and tracheoesophageal fistula are birth defects which affect the esophagus and/or trachea (the windpipe).
Gastroschisis is an opening in the abdominal wall in which the intestines come out usually to the right of the belly button (the umbilicus). The condition may cause the intestines to be irritated and not function well after a baby is born.
Hydrocephalus is a condition in which too much fluid builds up and puts pressure on the brain. Doctors commonly refer to hydrocephalus as “water on the brain.”
Intestinal atresias are intestinal blockages that may occur when there is not enough blood flow to the intestines as a fetus develops in utero.
Omphalocele is when a baby's abdominal wall doesn’t close and abdominal organs stick out of the base of the umbilical cord (belly button).
Spina bifida is a birth defect in which the spinal cord isn’t properly formed. This is a type of neural tube defect.
Trisomy 13 is a condition caused by an extra copy of chromosome 13. Having an extra copy of chromosome 13 causes the body to form differently.
Trisomy 18 is a condition caused by an extra copy of chromosome 18. Having an extra copy of chromosome 18 causes the body to form differently.
Twin to twin transfusion syndrome occurs when abnormal blood flow causes one identical twin in the uterus to not receive the necessary nutrients to grow from the shared placenta.
A urine blockage can develop while a baby is in the womb, preventing urine from passing out of the baby’s body.
-
Airway obstruction
-
Amniotic bands
-
Central nervous system abnormalities
-
Cystic hygroma/cervical teratoma
-
Fetal anemia and thrombocytopenia
-
Growth restriction
-
Hydrothorax
-
Lower urinary tract obstruction (LUTO) and other urologic abnormalities
-
Neck masses
-
Skeletal dysplasia
-
Sacrococcygeal teratoma (SCT) and other fetal neoplasms
-
Twin-reversed arterial perfusion (TRAP) sequence
Fetal Surgery and Intervention
Rapid advances in the field of fetal surgery make it possible to correct or manage certain life-threatening conditions even before a baby is born. Children’s Mercy cares for a growing number of moms and babies through fetal surgery each year.
Fetal Health Center Patient Family Advisory Council
The Fetal Health Center PFAC supports the highest standard of excellence in Fetal Health care at Children's Mercy through meaningful collaboration between families and hospital staff.
Stories
Against all odds: EXIT procedure helps baby Farrah start strong
A team of 40+ experts from the Children’s Mercy Fetal Health Center performed a unique prenatal surgery called an EXIT procedure to remove a large tumor that was pressing on baby Farrah’s lungs.
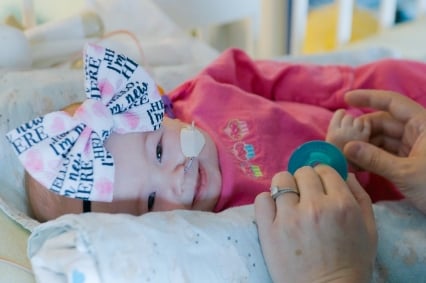
Prenatal Spina Bifida: Rose's Story
Taylor and James, business owners in Atlanta, faced a challenging pregnancy when their baby was diagnosed with hydrocephalus and spina bifida. Thanks to the swift and collaborative care at Children's Mercy Fetal Health Center, they received the necessary support and eventually moved to Kansas City, where Taylor joined the Fetal Health Center Patient Family Advisory Committee.

Fetal Heart Block: Reese's Story
Taylor and Caleb Jeter's unborn daughter, Reese, was diagnosed with fetal heart block while they were stationed in Germany. They were referred to Children's Mercy Kansas City for specialized care, where a multidisciplinary team managed Reese's condition and performed a successful surgery after her birth. Reese now has a pacemaker and continues to receive ongoing care and monitoring.
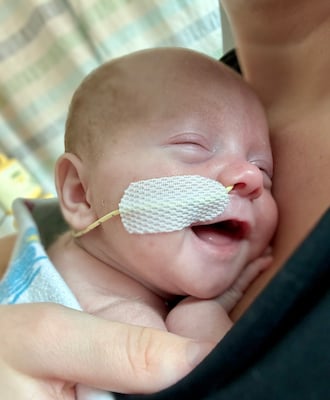
Fetal Health Center and NICU: Birdie and Erika’s Story
First-time mom Erika has been through a lot with her daughter Birdie. From delivering in our Fetal Health Center to several months in the NICU and multiple surgeries, Erika knows the hospital so well that she joined our staff! Read Erika and Birdie's story.

Fetal Health Center and NICU: Wisdom and Aisha's Story
Aisha’s faith, family and incredible care team at the Elizabeth J. Ferrell Fetal Health Center at Children’s Mercy carried her through three weeks of painful early labor, an emergency C-section delivery, and another three weeks in the Neonatal Intensive Care Unit (NICU) with her third son, Wisdom. Read their story.

Inside Pediatrics: Evelyn's story
Fetal surgeons at Children’s Mercy push the possibilities with a dramatic spinal repair surgery performed on baby Evelyn before birth.
Schizencephaly: Ajla and Audie's story
Diagnosed at 23 weeks with a rare brain defect, schizencephaly, Ajla and Audie Leonard have received the advantage of specialized care from a wide range of Children’s Mercy’s health experts.
The inspiration behind the Fetal Health Center
In 2010, Elizabeth J. and James E. Ferrell gave a generous gift that helped create the Fetal Health Center at Children's Mercy. In collaboration with the University of Missouri-Kansas City School of Medicine, the Center fosters local, national and international partnerships between researchers and physicians. Together, we are leading the way toward innovative treatment options for moms and babies.