Acute Lymphoblastic Leukemia: Munira's Story
Meet Munira

Munira Nuru is a proud Black Muslim woman. She presents every aspect of her identity through her appearance; from the hijab she wears as a symbol of her religious faith to the color of her skin.
But in 2018 Munira’s physical appearance began to change—not by choice, but because she had a life-threatening form of cancer.
Munira’s cancer journey began on Feb. 7, 2018, a few days before her 17th birthday. “I developed a high fever of 103 degrees Fahrenheit with a fever blister that lasted about a week. It was alarming because I had never had a fever before,” Munira said.
To try to get to the bottom of the problem, Munira went to the doctor. When a test for the flu, a likely explanation, came back negative, she just endured the fever until it eventually went away.
Another fever
About six months later in July 2018, the fever returned along with chills. This time Munira also had bumps, some the size of ping pong balls, on her face, scalp, neck and behind her eyes.
“The bumps changed the features of my face, which was very scary,” Munira said. “I started looking different. I was swollen and puffy. I looked like I had gained weight. I was anemic and exhausted, and my skin was pale. None of this was normal for me.”
In spite of multiple medical visits and tests, the cause of Munira’s symptoms remained a mystery.
“I started my senior year at Blue Springs South High School unsure of what was going on,” Munira said.
More doctor visits followed with a possible lymphoma diagnosis, but even that was unclear. Meanwhile, Munira was spending more and more time in the school nurse’s office, causing her to miss classes.
Then on Sept. 7, 2018, Munira was having difficulty breathing at school. “I have a history of asthma, but this was different,” she said. “It felt like someone was sitting on my chest. It didn’t matter what position I was in. I couldn’t breathe.”
Lifesaving decision
Munira called her mother to let her know about this new symptom. When her mom picked her up at school, she made a lifesaving decision for her daughter.
“I was 17, but my mom decided to take me to the Children’s Mercy Urgent Care near our house,” Munira said. “Everyone there was very responsive and attuned to what I was saying.”
After listening to her lungs and performing a chest X-ray, the doctor delivered disturbing news—her left lung had collapsed. “They wanted to rush me to the Children’s Mercy Adele Hall Campus. At that point, things began moving so fast.”
When she arrived at the hospital, doctors placed a chest tube to help drain the fluid around her lung and improve her breathing. Then Munira met Dr. Guest.
After more testing, Dr. Guest confirmed that Munira had B-cell acute lymphoblastic leukemia. “Dr. Guest is a very calm, tranquil individual and she truly helped settle a lot of my nerves,” Munira said. “The diagnosis was not desirable news, but ultimately, it was what I was expecting.”
Munira admitted she was scared, but relieved to finally know what was causing her symptoms. “Dr. Guest said there was a 90+ % success rate of treating this type of cancer, and she was confident I was going to be able to beat it.”
“Munira had a significant amount of fluid around her lung and her symptoms were advanced,” Dr. Guest said. “Because she was older than 10, we considered her high risk.”
To be certain Munira didn’t have any additional hereditary or tumor-specific risk factors, Dr. Guest performed whole genome sequencing on Munira’s cancer and healthy cells.
“An advantage of being treated at Children’s Mercy is that the Genomic Medicine Center sequences every child’s cancer in house using whole genome sequencing, the most comprehensive method available,” Dr. Guest said.
In Munira’s case, the sequencing didn’t reveal a hereditary link or characteristics that were driving the cancer, leading Dr. Guest to recommend a standard course of chemotherapy for her patient.
While still hospitalized on 4 Henson, Munira began her first treatment based on the most recent clinical trial results available.
In all, her therapy course involved a combination of in- and outpatient treatments over two years and two months. For the first nine months, she came in for weekly chemotherapy, then she graduated to monthly visits.
“Though Munira was almost an adult when she began treatment, research has shown the outcomes are better when adolescent patients are treated in a pediatric hospital,” Dr. Guest said.
When Munira finished her first round of treatment, her bone marrow was still positive for leukemia, but after her second round, the cancer was in remission.
Side effects
Over the next two years, including multiple hospitalizations, Munira experienced a number of treatment side effects, from headaches to peripheral neuropathy to a painful bacterial infection in her mouth and throat.
But probably her most significant side effect was a stroke-like syndrome induced by one of the chemotherapy drugs that was part of her treatment.
“That happened a few days before my 18th birthday,” Munira said. “I took a nap and woke up with facial droop and paralysis. I couldn’t move my face and my tongue felt fat.”
At the hospital, doctors performed an MRI to rule a stroke out, then determined the problem was related to the chemotherapy. Munira remembers the doctors adjusting her medication dosage and having her drink cough syrup to help the symptoms go away.
“The symptoms were only temporary, but it was nerve-wracking,” she said. ”Anytime I had an unusual side effect, the team would adjust and accommodate the medications for me. Their commitment to my care was great!”
During her treatment, Munira also required 30 units of blood and 14 units of platelets, both critically important to help keep her blood cell counts in a healthy range so that she could effectively fight the cancer.
However, one of the long-term issues the transfusions can cause is iron overload—too much iron can be damaging to vital organs, such as the heart and liver.
“We start to be concerned about iron overload after a patient has had more than 20 units of blood, which Munira did,” Dr. Guest said.
Fortunately, there is an effective treatment called chelation therapy, which uses a medication to bind to the iron and slowly remove it from the body in the urine. Munira will continue these treatments until her levels return to normal, plus she will follow up with her team regularly for lab work and scans until she transitions to adult care.
Treatment also sapped Munira’s strength and stamina. “During treatment, I lost a lot of my physical strength and flexibility, so after finishing my treatment, I have made it a point to regain that,” she said. “While it may seem like a simple task, becoming more active is such a gratifying goal for me because it means that I am making progress and getting closer to achieving my dream.”
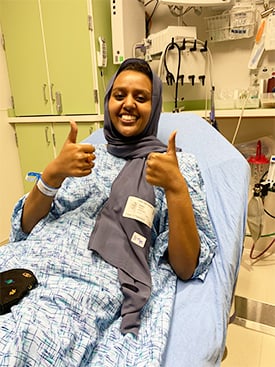
Though Munira has faced some significant obstacles during her cancer journey, with faith and grace, she has overcome each one. “There is a verse from our Holy Quran that says God does not burden a soul beyond what it can handle,” she said. And handle it, she did!
“Munira came to every treatment with a smile. Even though we knew she was struggling behind the scenes, she was always positive,” Dr. Guest said. “You could see her strength and we admired that.”
Now 20 years old, Munira has a promising prognosis. “The longer she stays in remission, the less likely it is that the cancer will return. At five years, we would consider Munira more than likely cured,” Dr. Guest said.
Silver linings
Before cancer became part of Munira’s journey, she was interested in a career in medicine. “In high school, I was on a pre-med track,” she said. With two older brothers who have also pursued careers in health care, Munira followed their lead, participating in the high school health club.
When her cancer treatment began, Munira said it was important to look for the silver linings anywhere she could find them.

“I am a determined individual who happened to be dealt a bad hand when diagnosed with cancer, but I was able to turn that into an opportunity to learn and grow by having faith that in the end, it will all work out,” Munira said. “I hope to always find the silver lining in the hardships I inevitably will face.”
Several of those silver linings came in the form of the relationships Munira formed with Dr. Guest and the Children’s Mercy Hematology/Oncology nursing team.
“Dr. Guest is incredibly knowledgeable and personable. It’s truly inspiring to hear her talk about her passion for medicine and her confidence in treating people. You can tell she loves to learn,” Munira said.
Assisting Dr. Guest with Munira’s cancer care was Paige Johnson, Advanced Practice RN II. “Paige is a fireball,” Munira said. “She is the personification of energy and just exudes it. She is the most helpful person I have ever met. She would encourage me to talk about how I was feeling, and helped connect me with important resources,” she added.
“All of my Children’s Mercy nurses were wonderful. I was there for so many weeks. Each of the nurses and caregivers made it a very comforting atmosphere,” she said. “They would sit and talk with me and distract me. If I needed anything, they would provide it for me. It was more like a friendship. Everyone at Children’s Mercy was incredible!”
New insight
In addition to her new-found friends, Munira gained valuable insight into her own future during treatment. “The medical insight and knowledge I gained first-hand is not something you can learn in academia,” Munira added. “The treatment was worth it if I can put it into practice in the future.”

And that’s exactly what Munira intends to do. After graduating from high school on schedule, she attended classes at Longview Community College and has now transferred to the University of Missouri-Kansas City where she’s pursuing a degree in biology. After that, she’s hoping to apply to medical school and to one day specialize in oncology.
“This experience and having Dr. Guest as my physician have changed my career path,” Munira said. “It gave me a sense of purpose and a role model to emulate,” she said.
When not studying, Munira describes herself as an avid reader, enjoying everything from poetry to fiction to philosophy. She also is determined to teach herself new skills, like writing with her left hand, or re-learning old ones, like jumping rope.
Because she’s faced discrimination and exclusion herself in high school, she has a special passion for the Black Lives Matter (BLM) movement.
“The adversities I have faced as a Black Muslim woman led me to become committed to social change,” Munira said. “BLM, in its purest form, is a call for action, and I find the movement inspiring as an individual who is actively trying to combat exclusion in my community and ensure positive impact.”
Dr. Guest has no doubt that Munira will achieve all her goals, and then some.
“It’s been a pleasure to care for Munira,” Dr. Guest said. “We are very supportive of her dreams and would welcome her back as a medical student one day. Because of her personal experience, she will be an amazing physician and advocate for her patients!”
Munira may take her up on that. “Children’s Mercy has set the bar for my whole life,” Munira said. “I now know what quality health care is, and I don’t think anyone should have to settle for less.”
Acute promyelocytic leukemia: Teo's story
Teo was diagnosed with acute promyelocytic leukemia (APL) and started treatment immediately. Thanks to a clinical trial, Teo was able to complete his treatment much more quickly and get back to the activities he loves.

- Cancer Center
- Cancer in Adolescents and Young Adults
- Brain Tumor Treatment
- Experimental Therapeutics
- Genomic Medicine in Cancer Treatment
- Histiocytosis Program
- Leukemia and Lymphoma Program
- Li Fraumeni Syndrome
- Liver Cancer Treatment
- Proton Therapy
- Soft Tissue and Bone Sarcomas
- Spanish-Speaking Cancer Clinic
- Surveillance for Predisposition to Tumors (SPoT) Clinic
- Survive & Thrive
- Cancer Center Family Care Team
- Hematology, Oncology, and Blood and Marrow Transplant
- Meet the Team