Rumination Disorder: Bobbi’s Story
Meet Bobbi
Just try keeping up with Bobbi Horr. The junior at Holton High School, Holton, Kan., is on the school’s spirit squad, in band, plays volleyball, runs track, takes dance and gymnastics, and works weekends waiting tables at the Trail’s Café.
She’s also enrolled in honors and advanced placement courses, like algebra II, language and composition, chemistry and American history.
Her goal is to be the absolute best at everything she does. No exceptions. But meeting such high standards can be stressful, sometimes causing health problems to surface.
Bobbi and her mom, Heather, said that’s what happened to her recently. Over the years, Bobbi had noticed that at stressful times, like the holidays or the beginning of the school year, she would have problems digesting her food. She would chew it up, but then wouldn’t be able to swallow it and would spit it out.
“We thought it was acid reflux at first,” Heather said. Bobbi agreed and said even when she was just 3 or 4 years old, when she was experiencing stress, like if her parents went out of town, she would have trouble swallowing her food, and would spit it back up.
“I would take some Tums to help, then when they got back home, it would stop,” she said.
But when Bobbi started her sophomore year of high school, the behavior became more severe. “I started spitting up everything,” she said. “I couldn’t even drink a glass of water.”
Bobbi tried to eat, but said she would feel bloated and uncomfortable. When her food would come back up, she would spit it in a cup, bottle or tissue and throw it away.
“It was embarrassing at school and disrupted class,” she said. “Sometimes I would have to get up and go to the bathroom to spit my food out, but I couldn’t help it. It made my stomach feel better.”
Concerned, Heather took Bobbi to the family’s primary care provider, who initially thought she might have acid reflux.
The doctor prescribed an acid-reducing medicine, but it didn’t help. After undergoing blood tests, a barium swallow test, and taking two more medications, Bobbi was still spitting her food up.
“Our doctor had tried everything he could think of, so he referred Bobbi to the gastroenterologists at Children’s Mercy,” Heather said.
Getting to the source of the problem
Bobbi’s first appointment at Children’s Mercy was a telehealth visit with John Rosen, MD, a pediatric gastroenterologist. As Dr. Rosen listened to Bobbi’s symptoms and reviewed her test results, Heather said he suggested Bobbi might have a rare condition called rumination disorder, not acid reflux.
Rumination disorder causes the backward flow of recently eaten food from the stomach to the mouth. The food is then re-chewed and swallowed or spat out. This typically happens immediately to 15 to 30 minutes after eating.
Rumination often occurs without retching or gagging. It may be proceeded by a feeling of pressure, the need to belch, nausea, or discomfort. Some people with rumination disorder experience bloating, heartburn, diarrhea, constipation, abdominal pain, headaches, dizziness, or sleeping difficulties.
Initially, it may be triggered by emotional distress, viral illness or physical injury. In many cases, no underlying trigger can be identified. The main treatment for rumination disorder is behavioral therapy. This may involve habit reversal strategies, relaxation, diaphragmatic breathing and biofeedback.
Dr. Rosen recommended diaphragmatic breathing as a first-line treatment for Bobbi and taught her how to use it during her telehealth visit. But at the next appointment, Bobbi said the breathing technique wasn’t helping relieve her symptoms. She was still spitting her food up and felt full after eating a small amount. That’s when Dr. Rosen prescribed an additional therapy called cyproheptadine, a medication to decrease the feeling of fullness, reduce stomach pain and potentially improve appetite.
When the medication didn’t help, Dr. Rosen referred Bobbi to the hospital’s new Rumination Disorder Clinic where she saw Jennifer Schurman, PhD, Associate Division Director of Integrative Care and Innovation; Chief, Section of GI Psychology; Director, Gastroenterology Research; and Co-Director, Abdominal Pain Program.
Dr. Schurman has been instrumental in developing the Children’s Mercy Gastroenterology Division’s unique biopsychosocial approach to care, addressing physiological and behavioral factors that may impact a patient’s gastrointestinal health.
The new Rumination Disorder Clinic is the only one in the region specializing in helping patients like Bobbi by offering a multidisciplinary approach to care, starting with a medical evaluation. Once any medical issues have been addressed, patients begin working on behavioral issues.
After talking with Bobbi, Dr. Schurman suspected stress might have triggered the disorder years earlier, but she had learned to suppress it. As she got older and faced even more stressful situations, the habit resurfaced, causing her to start spitting her food up again.
“Rumination disorder is probably more common than we think,” Dr. Schurman said. “When there is no medical cause for the problem, we focus on changing the habit or behavior.”
And that’s just what Dr. Schurman helped Bobbi do. At her first visit, Dr. Schurman explained that at some point, Bobbi’s esophagus had learned to push food up in response to stress, and that she needed to retrain those muscles to push food down instead.
She taught Bobbi breathing exercises to help her relax, and recommended she do them daily. Dr. Schurman also explained that even though it didn’t make Bobbi feel good, she needed to swallow her food, not spit it out. And, she suggested Bobbi try sucking on hard candy or a mint the first 30 minutes after eating, causing her to continuously swallow, another strategy to help retrain her esophagus.
During her first in-person visit, Dr. Schurman used biofeedback to determine how Bobbi responds to stress. Biofeedback therapy is a safe, painless technique where patients are trained to improve their health using signals from their own bodies.
Electronic biofeedback sensors were connected to Bobbi’s forehead and fingers to provide computerized information about muscle tension, hand temperature, and hand moisture levels. The biofeedback machine acted as a kind of sixth sense, allowing her to see or hear activity inside her body.
Dr. Schurman used the information gained from the biofeedback sessions to teach Bobbi additional skills to reduce stress, balance her nervous system, and reduce or eliminate physical symptoms.
“Bobbi was committed to changing this habit, and was a very compliant patient, making her treatment all the more effective,” Dr. Schurman said.
Gaining control...
Over the next six months, Dr. Schurman and Bobbi continued to meet every two weeks, sometimes in person, and sometimes virtually. They talked about school, stress, and how well the exercises were working to help her feel more in control of her body, and her life.
“I thought Dr. Schurman might tell Bobbi she needs to cut back on some of her activities or classes, but instead, she taught her how to manage the stress better,” Heather said. “She hasn’t had to cut back at all.
“We loved Dr. Schurman,” Heather said. “Before we were referred to Children’s Mercy, I was really worried about Bobbi. She wasn’t getting better and we didn’t know why. It just amazed me how well her treatment went.”
Now, with Dr. Schurman’s help, Bobbi said her life is returning to normal. She’s focused on her classes, and thinking about the future once she graduates from high school in 2022.
“There are so many things I want to do,” Bobbi said. “I’m interested in science and health and I love to cook. I want to go to college, but I’m not sure where.”
As Bobbi faces these new challenges, she knows there’s a possibility the rumination disorder could flare up again, but this time she’ll be ready for it.
“Dr. Schurman has taught me how to recognize my stress and has given me the skills I need to manage it,” Bobbi said. “Thanks to her, now I know what to do, and where to turn if I need help.”
Photo courtesy of Brian Nelson Photography.
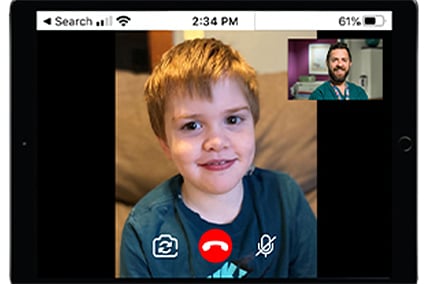
Delivering complex medical care via telemedicine: TJ’s story
Several complex medical conditions make visits to Children’s Mercy a challenge for TJ DeCow. Now, telemedicine visits are making it possible for TJ’s doctors to check in on him remotely, reducing his anxiety level, saving travel time to and from the hospital, and limiting time away from work for his mom.
Hypersensation of the gastrointestinal tract: Amarissa’s story
At 4 ½, Amarissa Hampton has struggled with painful constipation since birth. Finally, she was referred to the Gastrointestinal team at Children’s Mercy, and after a lengthy hospitalization, she’s doing better than ever. Now she’s enjoying her favorite foods, like ice cream and pizza, she has lots of energy, and she’s thriving for the first time in her young life.

- Gastroenterology
- Celiac Disease
- Constipation and Encopresis
- Feeding Clinic
- GI Procedures: What to Expect
- Inflammatory Bowel Disease
- Intestinal Rehabilitation Program
- Liver Transplant
- Pediatric Abdominal Pain Program
- Pediatric Gastroenterology Fellowship
- Pediatric Motility
- Rumination Disorder Clinic
- Meet the Team
Associate Division Director, Gastroenterology Integrated Care & Innovation; Section Chief, Gastroenterology Psychology; Co-Director, Abdominal Pain/Rumination Program; Professor of Pediatrics, University of Missouri-Kansas City School of Medicine