Hypersensation of the Gastrointestinal Tract: Amarissa’s Story
Meet Amarissa
Ice cream, popsicles, pepperoni pizza and fish sticks are just a few of 4 ½-year-old Amarissa Hampton’s favorite foods. But until just a few months ago, the tiny girl with the wispy light brown hair was rarely able to enjoy them.
Born Jan. 20, 2016 near her home town of West Fork, Ark., Amarissa’s mom, Ashley Malin, said her daughter’s birth seemed normal. Looking back now though, she had problems with bowel function from the very beginning.
“Amarissa was a week old before she passed her meconium, and it was very painful for her,” Ashley said. Typically this thick, green, tar-like substance is released in the baby’s first bowel movements shortly following birth.
Since then, Amarissa has struggled with painful constipation.
“Around 6 months old, Amarissa began having even more difficulty with her bowel movements,” Ashley said. “She was fussy, and wouldn’t eat. Meals were always a struggle. She would chew up her food and spit it out.”
By the time she was 18 months old, things were getting even worse. “We went to the pediatrician, but they just thought she had bad constipation,” Ashley said.
Laxatives and enemas didn’t help at all, and Amarissa continued to struggle—in pain, tummy distended, not gaining weight.
“She was a happy little girl, except when she needed to have a bowel movement,” Ashley said. “Then she was miserable.”
We’re going to Kansas City
Though Amarissa’s doctors referred her to specialists closer to home, a diagnosis continued to elude them. At 4 years old and only 23 pounds, Ashley knew her daughter was extremely sick, and she was desperate for answers.
Finally, a referral to Children’s Mercy gave Ashley hope that someone could help the preschooler before it was too late.
“Amarissa didn’t gain any weight between about 18 months and 4 years old,” Ashley said. “She was a very sick little girl when we got to Children’s Mercy.”
After the four-hour drive from their home, Amarissa arrived at the hospital late on Jan. 12, 2020. “With everything Amarissa had been through, she was scared to go to another hospital, but Children’s Mercy was a totally different experience for us,” Ashley said.
“Everyone at Children’s Mercy listened to me. They explained everything to be sure we were on board with what they were doing, and they made sure Amarissa was comfortable,” she said.
Shortly after being admitted to Children’s Mercy, Amarissa was assigned to the nursing unit on 6 Henson. Her gastrointestinal care team included Jose Cocjin, MD, Jennifer Colombo, MD, and William San Pablo, MD, all pediatric gastroenterologists; Rebecca Rentea, MD, a pediatric surgeon; and a group of nurses, residents and fellows, who all specialize in caring for children with gastrointestinal disorders.
In fact, the Division of Pediatric Gastroenterology at Children’s Mercy is one of the largest in the U.S. and is nationally recognized for providing excellent care for children with intestinal, liver, esophageal and nutritional disorders.
Children and teens with GI conditions benefit from the division’s comprehensive, child-centered care. Amarissa’s team focused on figuring out what was making her sick, and the best way to treat it.
First things first
The first order of business for Amarissa was to have a nasogastrointestinal tube and an IV line placed to help supplement her nutrition.
“During the first two weeks we were there, the team used total parenteral nutrition (TPN) to get Amarissa healthy again,” Ashley said. TPN is a way of supplying the body’s nutritional needs, bypassing the digestive system via the veins.
As she began feeling better and regaining her strength, Amarissa ventured outside her hospital room. She enjoyed doing arts and crafts and going to the play room on 6 Henson, playing bingo and going to pet pals.
As she regained her strength, her medical team searched for answers and solutions to Amarissa’s severe constipation, and failure to thrive.
“While 25% of our outpatient GI referrals are for constipation, Amarissa’s symptoms were severe and required multiple tests to gain a better understanding of what was happening to her,” said Jennifer Colombo, MD, pediatric gastroenterologist and one of Amarissa’s physicians.
Amarissa’s GI manometry, or motility studies, which test the function of her GI tract (how the muscles and nerves interact) were normal. According to Dr. Colombo, it seems that she has hypersensation of the GI tract. Her bowels worked until waste reached her colon, then they seemed to stop.
“Testing showed Amarissa has all the right muscles and nerves, but her nerves sense and interpret normal movement of the GI tract as severely painful, making it difficult to move the digestive waste through her intestines,” Dr. Colombo explained.
To help her consistently have bowel movements, the GI team recommended Amarissa have an ileostomy, a cecostomy and a feeding tube.
An ileostomy is an opening in the belly wall where the end of the ileum, or the lowest part of the small intestine, exits the body. Intestinal waste passes out of the ileostomy and is collected in an artificial external pouching system adhered to the skin.
A cecostomy is a small plastic tube that goes straight from Amarissa’s skin into the beginning part of the large intestine or colon. This creates a direct opening to the intestines, allowing them to be cleaned out daily, or flushed.
A feeding tube was inserted into Amarrisa’s stomach through the abdomen and is used to supply nutrition when she has trouble eating.
After spending six weeks in Children’s Mercy, including her fourth birthday and Valentine’s Day, she was finally able to head home on Feb. 19, 2020.
Amarissa was now healthier than ever—having gained seven pounds during her hospital stay. “When we got home, she had outgrown all of her clothes and shoes,” Ashley said.
Long live Amarissa!
Though Amarissa did well during the first few weeks back home, in April she began experiencing problems moving her bowels again. After a short stay in Children’s Mercy, doctors were able to help relieve her constipation. They also used Botox injections to relax her anal sphincter muscle, helping her to pass waste.
Ashley said this is the first time in her young daughter’s life that she’s been healthy, and she’s thrilled.
“When we first came to Children’s Mercy, I just wanted to find out what was wrong and do whatever necessary to fix it,” Ashley said.
“When the team told me what they wanted to do, it hit me like a load of bricks, thinking of all the things that she was going to be going through. But at the same time, that’s what saved her life. I am happy with the outcome.”
Back home now, Amarissa has lots of energy—even her voice sounds brighter. “She doesn’t sound weak. She sounds like a healthy little girl,” Ashley said.
Going forward, Amarissa will continue routine visits with her Children’s Mercy GI team. Ashley said the plan is for her to begin pelvic floor therapy to help her become more comfortable with her treatment routine and to strengthen her pelvic muscles.
“When we arrived at the hospital, Amarissa was gravely ill,” Ashley said. “She’s actually hungry now, eating three meals a day, plus snacks, and she’s more active than ever. She goes non-stop.”
“Amarissa is doing well and thriving,” Dr. Colombo said. “She comes to Children’s Mercy for check-ups. She has had a few procedures and still requires medications to help her colon function better. She has a long way to go, but she is a happy little girl. Everyone on Amarissa’s medical team is cheering for her.”
Ashley said the care Amarissa received at Children’s Mercy was exceptional. “She became best friends with her nurses. They would come and play with her. She still talks about them.”
And the physicians were great, too. “They all would tell you what their plans were, and would ask me about my concerns. They always wanted to know how our family felt, especially when it came to something Amarissa might not be comfortable with. If that was the case, they found another way.
“I would recommend Children’s Mercy to anyone whose child needs advanced GI care,” Ashley added. “They saved Amarissa. I think she’s going to have a long and happy life!”
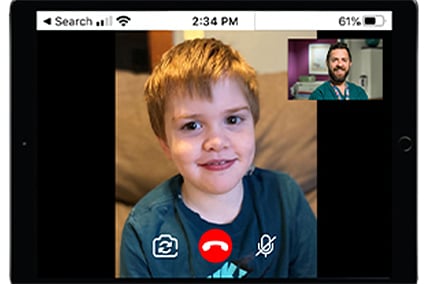
Delivering complex medical care via telemedicine: TJ’s story
Several complex medical conditions make visits to Children’s Mercy a challenge for TJ DeCow. Now, telemedicine visits are making it possible for TJ’s doctors to check in on him remotely, reducing his anxiety level, saving travel time to and from the hospital, and limiting time away from work for his mom.
Peutz-Jeghers syndrome: Toby's story
A rare genetic condition causes polyps to continually form in Toby Nguyen’s intestines. But thanks to the Children’s Mercy Polyposis Center and a unique test called double balloon enteroscopy, it’s under control.

- Gastroenterology
- Celiac Disease
- Constipation and Encopresis
- Feeding Clinic
- GI Procedures: What to Expect
- Inflammatory Bowel Disease
- Intestinal Rehabilitation Program
- Liver Transplant
- Pediatric Abdominal Pain Program
- Pediatric Gastroenterology Fellowship
- Pediatric Motility
- Rumination Disorder Clinic
- Meet the Team
Section Chief, Gastroenterology; Professor of Pediatrics, University of Missouri-Kansas City School of Medicine; Clinical Professor of Pediatrics, University of Kansas School of Medicine
Division Director, Gastroenterology, Hepatology & Nutrition; Professor of Pediatrics, University of Missouri-Kansas City School of Medicine; Clinical Assistant Professor of Pediatrics, University of Kansas School of Medicine
Director, Intestinal Rehabilitation Program; Assistant Director, Nutrition Support Service; Associate Professor of Pediatrics, University of Missouri-Kansas City School of Medicine; Clinical Assistant Professor of Pediatrics, University of Kansas School of Medicine
Section Chief, Colorectal & Pelvic Reconstructive Surgery; Medical Director, Colorectal Surgery & Comprehensive Colorectal Center; Program Director, Pediatric Surgery Fellowship; Professor of Surgery, University of Missouri-Kansas City School of Medicine