Hirschsprung Disease in Children
What is Hirschsprung disease?
We're here to help
To learn more about the Colorectal Center, complete this brief form and our team will get in touch with you, or call us at (816) 234-3441.
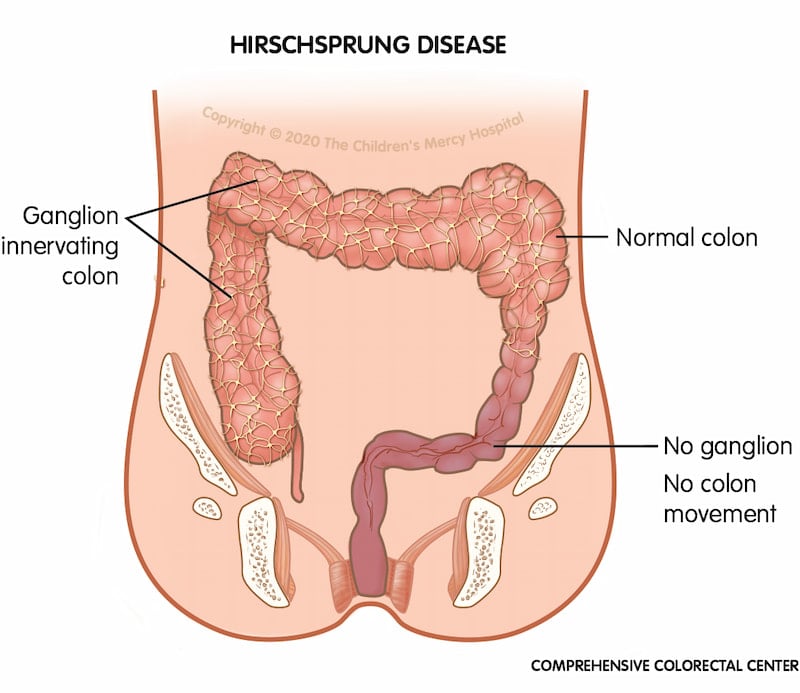
Hirschsprung disease (also known as congenital aganglionic megacolon) is a birth defect in which the end of a child's bowel does not contain all of the typical nerve cells, called ganglion cells. It also may affect the length of the bowel. The condition occurs in approximately one in 5,000 newborns and is more common in boys than girls. Children with other medical conditions, such as Down syndrome, are at a higher risk of having Hirschsprung disease. Hirschsprung disease appears to be hereditary in some cases, however the main cause isn’t entirely clear.
The lack of nerve cells along the bowel in a child with Hirschsprung disease prevents food and waste from moving forward through the colon to the anus, causing problems passing stool. Because of the lack of ability to sense when stool needs to be passed, the bowel does not relax. This can result in blockages, which can lead to damage within the bowel. For children with Hirschsprung disease, bowel movements can be difficult to pass even after surgery and toilet training may also be a challenging process.
Symptoms and diagnosis of Hirschsprung disease
Constipation, or not passing stool in the first 48 hours of life, is the main symptom of newborn babies with Hirschsprung disease. Other symptoms include vomiting green or brown vomit, swelling of the belly, the passing of a lot of gas, and bloody diarrhea. In milder cases, the condition might not be diagnosed until later in childhood. Rarely, Hirschsprung disease is first diagnosed in adults.
Three imaging tests are commonly used to diagnose Hirschsprung disease. There are:
- Contrast enema—this X-ray shows the doctor the part of colon that is diseased. Results help in planning for surgery.
- Rectal biopsy—the doctor removes a small sample of tissue from the last part of the colon (the lowest part of the large intestine) and looks for the ganglion nerve cells under the microscope.
- Anorectal manometry—this special test uses a small balloon to look for pressure changes in the colon and rectum. Usually, it is used for older children.
Treatment for Hirschsprung disease
Children’s Mercy is home to one of a very few Comprehensive Colorectal Centers in the nation. We take a team-based approach to care for children with colorectal malformations such as Hirschsprung disease and other anorectal and pelvic floor disorders, such as imperforate anus/anorectal malformation or cloaca).
Patients with anorectal and pelvic malformations may need many medical or surgical interventions during their lifetime. One of the first surgeries a baby or child might have is an ostomy surgery, which allows waste (poop) to leave the body through a hole in the abdomen (stoma). The poop is then collected in a bag. A multidisciplinary approach can reduce surgical interventions, anesthetic procedures, endotracheal intubations and, hospital/outpatient visits.
Call for an appointment
We're here to help you. Contact us for more information about the Comprehensive Colorectal Center at Children's Mercy.
Easing symptoms with rectal irrigation
Rectal irrigation can get rid of waste and keep the child’s colon healthy until surgery can be performed. Irrigation is done by inserting a tube into the child’s anal opening and flushing the colon out slowly. This can get rid of the waste and gas that are making the child sick and provides immediate relief.
When appropriate, parents also may be taught rectal irrigation and other methods to potentially ease symptoms at home.
How to Perform Rectal Irrigations
Hirschsprung disease can cause your child to have a backup of stool and gas in their colon. This can make them ill and struggle to have a bowel movement. However, there are a few steps you can take that will help keep your child’s colon clean. The Colorectal Center has provided this video as a visual resource for families who need to perform rectal irrigations at home.
Pull-through surgery
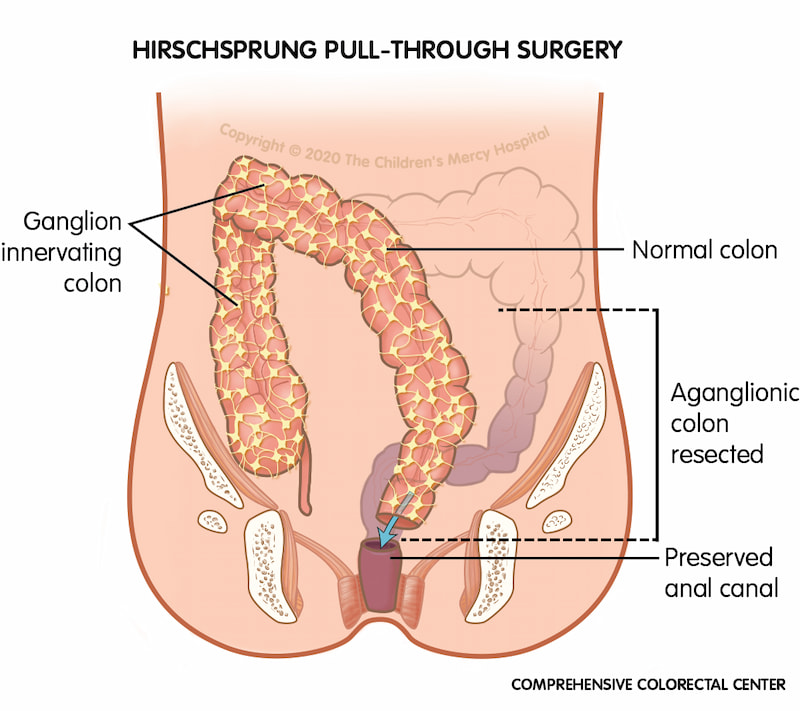
While rectal irrigation may provide temporary relief, the primary treatment for Hirschsprung disease is surgery to remove the portion of the colon without any nerve cells. This is called a pull-through procedure, or the Swenson procedure.
This procedure is usually performed when the child is first diagnosed with Hirschsprung. The physician takes tissue samples of the bowel, called a biopsy, to determine the areas of the colon that lack the nerve or ganglion cells. After the diseased portion of the colon is identified, the surgeon removes it and connects the healthy bowel to the child’s anus, allowing stool to pass.
As with any surgical procedure, there are risks to pull-through surgery. These include bleeding, infection, blockage of the bowel, constipation, incontinence and healing issues at the site of the pull-through.
What are the benefits of pull-through surgery?
There is no cure for Hirschsprung disease, but the Swenson procedure, or pull-through surgery, is the best way we know to help your child have bowel movements, or poop from their bottom instead of having to use a colostomy bag to poop.
Are problems common after pull-through surgery?
While surgical outcomes are generally excellent after pull-through surgery, Hirschsprung-associated enterocolitis (HAEC), or enterocolitis, is an inflammation of the colon that can occur. Enterocolitis can happen before or after surgery and can make your child very sick. Enterocolitis is usually treated with antibiotics and rectal irrigation.
Please always call your doctor’s office immediately if your child has Hirschsprung disease, or has recently had pull-through surgery, and you suspect an infection.
Symptoms of enterocolitis include:
- A swollen tummy
- Bleeding from the bottom
- Diarrhea, especially foul-smelling
- Fever
- Lack of energy
- Vomiting
Constipation is another common problem that many children have after pull-through surgery. Constipation usually can be managed with medicines and laxatives.
Your surgeon and the team at the Comprehensive Colorectal Center are experienced at assessing and managing issues following pull-through surgery. This may require an examination under anesthesia with additional studies and testing. Sometimes a redo-surgery is recommended. During this evaluation we will determine:
- Previous surgery performed (Soave, Swenson, Duhamel)
- Current anatomy
- Length of the colon
- Blockages to current anatomy (strictures, cuffs of scar tissue)
- Condition of the sphincters
- Condition of the nerves of the colon
These complex surgeries are best done with the help of a multidisciplinary team such as the one available at the Comprehensive Colorectal Center at Children’s Mercy.
How is Hirschsprung disease managed long term?
Bowel management is a clinical experience in which we work to empty the patient's bowels and colon. This experience may be managed in one of three ways:
- Outpatient clinic visits
- Inpatient stay
- One-week intensive outpatient experience called Bowel Management Bootcamp
These programs are available for children of all ages who are unable to anticipate or control their bowel activity. This experience is tailored to help patients resume normal bowel activity.
- Colorectal Center
- Speak With Our Team
- Comprehensive Colorectal Care
- Conditions and Treatments
- Bowel Management Boot Camp
- Colorectal Surgery
- Resources for Caring for Colorectal Conditions at Home
- Insurance Information
- Advancing Care Through Research
- What to Expect
- Meet the Team
- General and Thoracic Surgery
