Rumination Disorder: Austin's Story
Meet Austin

Eleven-year-old Austin Hasenohr excels at special-effects makeup. He also makes stop-motion animation movies and cartoon drawing animation on his phone, is accomplished at needle felting and practices jazz, ballet and contemporary dance.
And while he enjoys all these activities for their own sake, these days they also have become some of the ways Austin is learning to manage rumination syndrome, a troubling gastrointestinal disorder that a year ago landed him in the hospital and threatened both his physical and psychological wellbeing.
Rumination syndrome causes people to repeatedly, and unintentionally, regurgitate undigested or partially digested food shortly after eating or drinking as a result of dysregulated communication between the brain and GI system. It’s often initially prompted by a viral illness, allergy, nerve sensitivity in the GI tract, food poisoning or stress, but continues even after the triggering event passes. It’s involuntary, not widely understood, and sometimes mistaken for acid reflux or an eating disorder.
And while it doesn’t generally lead to physical damage, it can disrupt nutrition – and wreak psychological havoc on the lives of affected children and their families.
That was certainly the case for Austin, until a multidisciplinary team of medical and behavioral health professionals at Children’s Mercy worked with him and his family at the recently opened Rumination Disorder Clinic. The team treated the underlying gastrointestinal issues Austin was experiencing and helped him manage his body’s involuntary response - turning despair into determination.
A protective response in overdrive
Normally, wave-like contractions in the esophagus push food from the throat to the stomach for the next step in the digestion process. But with rumination, the waves move in reverse, gently bringing food back up before it reaches the stomach. It’s the body’s effort to alleviate pain or pressure downstream, according to Rumination Clinic Clinical Psychologist Jennifer Schurman, PhD, ABPP, BCB.
“If you have inflammation in part of your small intestine, for example, it’s like a rash, and your body doesn’t want to send food over that area because it’s irritated and will hurt, so it holds the food, causing pressure and pain that is relieved by sending it back up,” she said. “The way I explain it to kids is that, for whatever reason, their body has learned that it feels better, at least temporarily, to relieve pressure in their stomach by having the food come back up, kind of like a release valve.”
That’s all well and good if regurgitation stops once the inflammation is gone, but it becomes a chronic issue if the body, having now learned how to avoid discomfort, makes it an involuntary habit whether it needs to or not.
“Rumination is your body saying, ‘hey, this worked before, I’m going to do it again,” Dr. Schurman said. “Our bodies are meant to protect us, and this is one way it’s trying to do that. But it’s trying to do its job too well.”
That’s what happened to Austin.
‘There’s something more’
Shortly after the Christmas break from school last year, Austin became sick – unable-to-keep-anything-down sick.
“He’d sit with a bucket, take a bite, and have to spit it back out, 30 to 50 times a day,” said his mom, Tiffany Hasenohr.
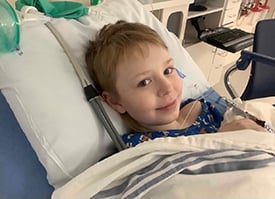
Miserable and becoming malnourished, he was hospitalized for a week and diagnosed with inflammation of lymph nodes in a membrane attached to his abdominal wall. But Tiffany was unconvinced.
“I kept telling the doctor, ‘there’s something else wrong.’ I just knew in my soul, there’s something more,” she said.
After Austin was released from the hospital, Tiffany drove her son from their home in Hiawatha, Kansas, to Children’s Mercy in Kansas City. He was referred to a CM gastroenterologist who confirmed the earlier diagnosis but also listened to Tiffany’s insistence that there was more to the story, and ordered a scope of his esophagus, revealing eosinophilic esophagitis (EoE), a chronic inflammatory immune response to allergens.
Medication for heartburn, antihistamine for the allergic reaction and eliminating dairy and gluten from Austin’s diet helped him feel better, but the regurgitation continued. That’s when rumination was mentioned as a possibility, and once an additional scope indicated the EoE was in remission, he was referred to Dr. Schurman to help him manage what by then had become his body’s habitual response.
“Once the triggering physical event has passed, I’ll work on habit reversal to let the body know that having a little pressure in your stomach is safe and it doesn’t have to do this anymore,” Dr. Schurman said. “But we want to be sure we treat the medical issue first before we start asking patients to do the hard work around habit reversal, or they will still be vulnerable.
“That’s why it’s important to have a multidisciplinary approach to treating rumination.”
Competing response
What goes up must come down. That’s the idea behind one of Dr. Schurman’s body-retraining tactics: competing response.
“What I’ll recommend for kids to get some symptom relief and start to train their bodies to keep food down is sucking on something like a mint or hard candy for 30 to 60 minutes after eating,” she said. “Because if you’re doing that, you’re continuously swallowing, suppressing the reverse wave from happening and giving your body time to start to digest and send that food on, so there’s less pressure.”
Chewing gum, re-swallowing the returned food or brushing teeth may work, too.
“And I’ve had kids for whom singing or debate is a good competing response, because if you’re singing or giving a speech, you’re controlling your diaphragm and airway, so it’s harder for those waves in the esophagus to get traction.”
Singing didn’t work for Austin, but sucking on Jolly Ranchers did, as did stress-management techniques teaching him to calm his autonomic nervous system.
“Our bodies are always somewhere along the spectrum of ‘rest and digest’ or ‘fight or flight,’ and when you have a meal, you should be in rest and digest moving food down,” Dr. Schurman said. “But kids who are really stressed and constantly in a state of fight or flight will have a harder time moving things downstream because their body thinks it’s an emergency.”

Biofeedback, allowing patients to visualize and then calm stress reactions with diaphragmatic breathing, progressive muscle relaxation or other tactics, is helpful for some children, as is diffusing stress with other activities. Austin has become proficient at both, and is where Austin’s creative pursuits – dancing, creating cartoon animations and movie-worthy faces with special effects makeup or assembling a plush character with needles and scraps of felt – have come into play.
“He’s always been the type of person who likes his schedule, likes to know what to expect, so rumination really threw him back,” Tiffany said. “But we’re now at a point where he says, ‘OK, I can control this, I can make the choice to calm down.’
“It’s fun to watch, because I see his whole body relax. His mind is so busy that he can’t do rumination anymore,” she added. “And I’ve had people comment that he’s like a whole new kid now.”
Don’t give up

Rumination can be embarrassing, socially isolating and psychologically distressing for kids. There were times, Tiffany recalled, when Austin became so tired of spitting into his bucket, he was ready to give up.
And the work to keep it at bay is hard, sometimes unpleasant, requiring trial and error to determine what works for each child, then patience and consistency over time. New stresses – like the flu or other illness, or school and family disruptions – can bring on relapses.
But it’s well worth the effort, because the right combination of individualized support from a multidisciplinary team of professionals who can address both the physical and psychological effects of the condition make it possible for kids to get it under control and keep it under control for the long term.
And that brings Austin joy, along some advice for others who experience rumination: Don’t give up. You can do this.
Rumination disorder: Bobbi’s story
Seventeen-year-old Bobbi Horr was referred to Children’s Mercy when she was unable to swallow her food and began spitting it up constantly. The Gastroenterology team diagnosed her with rumination disorder, a rare syndrome often caused by stress. Thanks to behavioral modification, Bobbi has learned how to effectively manage her stress, and continue her active life as a junior at Holton High School.

- Gastroenterology
- Celiac Disease
- Constipation and Encopresis
- Feeding Clinic
- GI Procedures: What to Expect
- Inflammatory Bowel Disease
- Intestinal Rehabilitation Program
- Liver Transplant
- Pediatric Abdominal Pain Program
- Pediatric Gastroenterology Fellowship
- Pediatric Motility
- Rumination Disorder Clinic
- Meet the Team
Associate Division Director, Gastroenterology Integrated Care & Innovation; Section Chief, Gastroenterology Psychology; Co-Director, Abdominal Pain/Rumination Program; Professor of Pediatrics, University of Missouri-Kansas City School of Medicine