Bariatric Surgery Program
The highest level Children's Surgery Center available

Weight loss surgery may be an option for teens and young adults who have tried medically-supervised weight loss programs but still struggle with obesity.
Obesity is a medical condition and surgical weight loss can be a life-saving treatment. However, it’s important to understand that surgery is not a “quick fix,” but part of a lifelong commitment to a healthy lifestyle.
The bariatric surgery program at Children’s Mercy begins by working together to evaluate if surgery is the best option for you. We find that this treatment option is most successful for kids and teens who:
-
Are at least five years old
-
Have a BMI of at least 40 (or above 35 if other medical conditions like type 2 diabetes, sleep apnea, fatty liver disease or others are present)
-
Have had at least 6 months of supervised medical weight loss therapy, including dietitian and psychological evaluations
-
Are ready to make long-term changes to their diet and exercise habits
How does bariatric surgery work?
At Children’s Mercy, we perform a minimally-invasive type of bariatric surgery called a laparoscopic sleeve gastrectomy. Your surgeon will use a small, flexible camera and special tools to remove a large portion of your stomach, including the part that produces the hunger-inducing hormone ghrelin. That way, when you eat, you feel full sooner.
This kind of surgery only requires small incisions in your abdomen, so most people won’t have any big scars. Laparoscopic surgery also has a shorter recovery time and fewer risks than open surgery.
A lot of insurance companies will sometimes pay for bariatric weight loss surgery. A member of our team will be glad to help with your insurance questions.
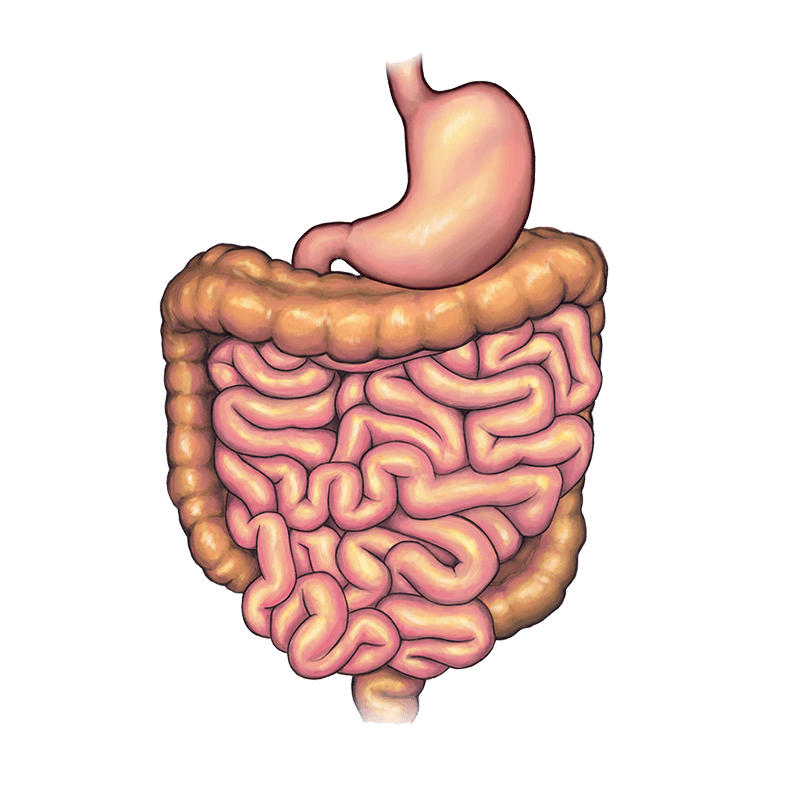
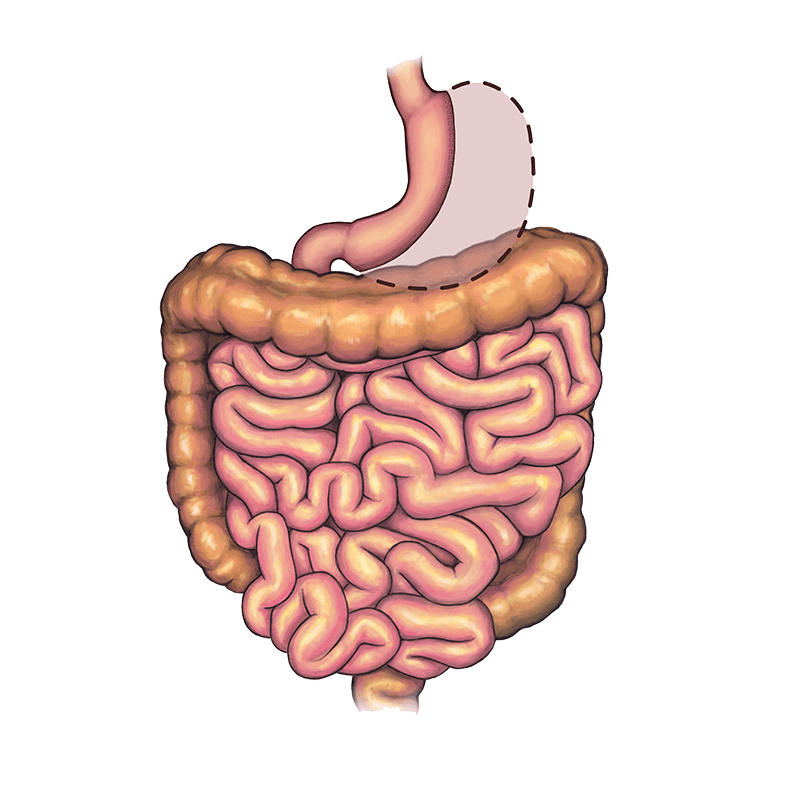
Recovering from gastrectomy
After surgery, you will most likely stay in the hospital overnight or until your doctor feels you are well enough to recover at home. It will take several weeks for your stomach to heal from the surgery, so your diet will be very different for a while as your body adjusts. We will be with you every step of the way to help you succeed.
Weight loss surgery is a lifetime commitment. Your surgeon will recommend a schedule for visits based on your surgery and health care needs. Even after you reach your goal weight, your medical team will still monitor your health.
Gastric sleeve: Long term-effects
Even when you’re feeling better, you should know that weight loss surgery is a lifetime commitment. You will need to have follow-up appointments with your medical team and learn healthy eating habits that will help you maintain your weight even after you’ve reached your weight loss goals.
The weight management team at Children’s Mercy works with kids and teens every day. It’s a good idea to spend some time talking with your doctor and your family about how weight loss surgery will affect you in the long term. There are some topics that may not be of concern to you now, but can have a significant impact on your adult life. Part of your care plan will be helping you prepare for these moments so you know how to handle them when the time comes.
For instance, studies have shown that teens with severe obesity who underwent stomach reduction surgery to lose weight also significantly improved their heart health.
Also, as an adult, you will have to be very careful about consuming alcoholic beverages. Your doctor may recommend that you drink only small amounts of alcohol, or avoid it altogether, depending on your circumstances.
Another area for girls and women to consider is the impact of weight loss surgery on your fertility, or ability to get pregnant. Infertility—difficulty getting pregnant—can often be a complication of obesity. Many women experience a positive change in their fertility after bariatric surgery, where their menstrual cycles become more regular and they’re more likely to conceive. This may mean you need to think about birth control if you do not want to become pregnant.
Our weight loss surgery experts
Children's Mercy is the only hospital in the region with a fellowship-trained pediatric surgeon who performs the gastric sleeve operation. The surgical team also includes fellowship-trained pediatric anesthesiologists, as well as pediatric nurses and other support staff, including dietitians, social workers and psychologists. They are all experts in taking care of children and teens.
Enhanced recovery after surgery (ERAS)
Enhanced recovery after surgery (ERAS) is a pathway your child will follow for their upcoming surgery. This is a combination of practices that your child’s entire health care team will use to make sure they have the best care before, during and after surgery.
The ERAS pathway helps your child by:
- Educating your child and family during your clinic visits before surgery.
- Reducing the amount of time your child has to stop eating and drinking before surgery.
- Using non-opioid medications as the first course of treatment for pain, with opioids as the last option.
- Preventing nausea and vomiting after surgery.
- Getting out of bed and moving early after surgery.
- Drinking and eating early after surgery.
- Reducing complications after surgery such as nausea, constipation, pain, etc.
- Going home from the hospital sooner after surgery to allow your child to recover at home rather than in the hospital, when appropriate.
As a key part of your child’s health care team, you will be able to learn about the ERAS pathway during your visits with the surgical team. We encourage you to ask questions and let your child’s care team know if you have information about your child’s specific needs that might help with their recovery.
Gastric sleeve ERAS pathway for health care providers
The gastric sleeve ERAS pathway was developed in collaboration with the Department of Evidence Based Practice, Department of Pediatric Surgery, and the Department of Anesthesiology. The pathway, along with other evidence based products, can be found on our website.
Bariatric surgery: Lane’s story
When Lane was 17 years old and unable to lose weight through diet and exercise alone, he decided weight loss surgery was his best option. Through the Bariatric Surgery Program at Children’s Mercy, Lane lost over 200 pounds and continues to pursue a healthy lifestyle following his life-changing surgery.
Anesthesia
At Children’s Mercy, a pediatric anesthesiologist is an active member of your care team before, during and after your surgery or procedure. We administer anesthesia for more than 27,000 kids per year—that’s 74 per day—so our team is experienced at finding just-right doses of medication for kids of all sizes. During the procedure, your anesthesiologist will carefully monitor your heartbeat, blood pressure and breathing. Afterwards, your anesthesiologist will make sure you wake up as comfortably as possible and continue to help with pain control.
Contact us
There are a lot of things to think about before you decide to have weight loss surgery. Your pediatrician, primary care doctor and nurse practitioner may refer you to the Children's Mercy Surgical Weight Loss Program for more information.
Or, call the Children's Mercy Surgery Clinic at (816) 234-3199 to schedule an evaluation for weight loss surgery. We would be happy to answer your questions.
