Kidney Transplant Then & Now: Morea’s Story
Meet Morea
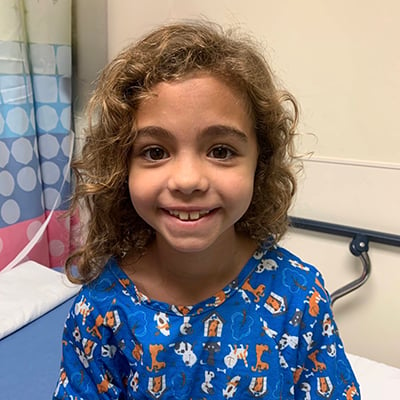
Morea is 15 and looking forward to the freedom an unrestricted driver’s license will bring her soon. Her childhood kidney transplant is in the rearview mirror; so far past, the memories are turning hazy. She’ll celebrate her kidney’s 9th birthday this coming September. Until then, this multi-style dancer (ballet, tap, jazz, lyrical, hip hop) has competition season, recitals, dance team and a whole summer vacation to savor — water bottle always in tow.
A virus led to an early diagnosis
Morea’s mom, Cameo, recalled the early days of their kidney journey, which started when Morea was just 7 weeks old. Cameo and Joe, Morea’s dad, were concerned when Morea caught a virus and began losing weight. Morea's pediatrician referred her to Children’s Mercy, where her care team also found high levels of protein in her urine. She recovered in the hospital, then followed up with Nephrology. A kidney biopsy and genetic testing revealed Morea had congenital nephrotic syndrome caused by a rare genetic variant.
“When babies are born with congenital nephrotic syndrome, the kidneys lose protein in the urine, leading to several complications, including low blood protein levels, swelling, increased infections and decreased kidney function with time,” said Heather Morgans, DO, Morea’s current nephrologist in the Brendan Tripp Elam Transplant Center at Children’s Mercy.
Morea's Nephrology and Transplant Center care teams were initially able to manage her condition with medications. When her declining kidneys led to nausea and lack of appetite, she had a feeding tube placed. By the time Morea was 5 and a half, she was in stage five chronic kidney disease, also known as end stage kidney disease. She needed a kidney transplant and began peritoneal dialysis at home while she waited for a donor.

“Peritoneal dialysis uses the capillaries in the peritoneum, the lining of the abdomen, to filter out waste products and extra fluid overnight,” explained Dr. Morgans. Dextrose in the dialysis fluid helps to remove the fluid and waste products through diffusion. A peritoneal dialysis machine is used to fill, dwell, and drain the fluid in cycles, usually 8 to 12 per night.
“I remember being very tired, and I couldn’t move around a lot,” said Morea of this difficult time. She would wake up in pain at night and could only make it through a half-day of school before needing a nap. She didn’t have energy to dance, something she had loved since she was 3 years old.
Cameo said Morea’s care team was amazing during dialysis and checked in daily, even on weekends. Another bright point: Morea’s little brother, Brecken, was born healthy in early 2017. He was “along for the ride” as the family prepped for Morea’s transplant.
Searching for a donor
Morea went on the active kidney transplant list in December 2016. People who need a kidney transplant can have a living donor or be listed for a deceased donor kidney — sometimes both, if the living donor evaluation is not yet completed.

Living donors need to meet age and health requirements, match the recipient’s Human Leukocyte Antigen (HLA) and have blood types that will mix well. Unfortunately, none of Cameo’s family members were able to donate.
As they waited for a donor, Morea’s blood pressure became harder to control.
“When your kidneys are functioning poorly, alterations of the renin/aldosterone system can lead to increased blood pressure,” said Dr. Morgans. “Removing those kidneys can help control blood pressure.”
Morea had a double nephrectomy to help manage her blood pressure and create more room to accommodate a larger donor kidney, if one became available. After the operation, Morea needed longer peritoneal dialysis treatments for about 10 days before returning home.
Finally, in September 2017, there was a kidney for Morea.
“We got the call on a Friday morning at 1 a.m.,” remembered Cameo. “They told us to go ahead and send her to school that day, and then mid-morning they called to say, ‘Everything’s good. Bring her in!’”
Life with one kidney
Morea's transplant and post-op recovery went smoothly. She adapted to her immunosuppressants well and had regular lab work and follow-up clinic visits that tapered down as her health improved. A port made Morea’s blood draws easier until she outgrew it around age 11, and she now comes to Kidney Clinic just four times a year.

After the transplant, her appetite returned, and she didn’t have to follow a restricted diet, like she did while on dialysis. “When I could eat whatever I wanted, I really liked to eat cheese,” Morea grinned. She loved string cheese so much, Cameo had said they had to start cutting off her cheese supply!
Like many young transplant patients, Morea's growth had slowed to a standstill while waiting for her kidney. Growth hormones after transplant helped her catch back up. “Here we are today, eight and a half years and lots of blood draws, procedures and biopsies later,” said Cameo. “It’s been very successful.”
“She has had a very good post-transplant course, and that is really all her doing: drinking her water, taking her medicines and just being a wonderful kid,” agreed Dr. Morgans.
“Dr. Morgans is very knowledgeable and is wonderful at listening to Morea's concerns,” said Cameo. “You can tell she really wants to get to know her patients and cares about their health and success.”
Solid organ transplant coordinator Katelyn Walser, RN, BSN, CPN, CCTC, joined Morea’s team in 2019. “It’s been so fun to watch her grow up,” said Katelyn. “She’s just the model patient. When she comes for kidney clinic, she knows all of her meds — the names and the doses and everything she takes, which is impressive.”
At her clinic visits, they check her labs, address any issues, go through medications and support Morea as she takes more responsibility for her health.
“Morea is really starting to come into her own and be more independent,” said Katelyn. Cameo said Katelyn has been an incredible support for their family and a great mentor for Morea as she approaches her transition to adult care.
“It’s expected that Morea will need another kidney transplant at some point,” said Dr. Morgans. “The average transplanted kidney will last 10 to 20 years. As medications improve and advancements come along, hopefully that will extend longer, especially for Morea. She’s done great, and her kidney function is still very good.”
“We know people who’ve kept their [transplanted] kidneys for 30 to 40 years, so we just hope for the best,” said Cameo. “We live every day to the fullest ... we just keep trekking forward.”
Summer, freedom and friends
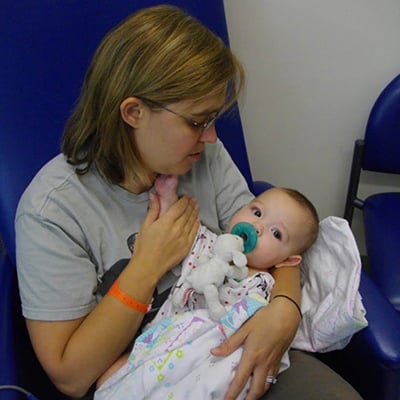
Cameo said strong relationships helped her family when they were in the middle of Morea’s transplant process. She tells other parents to build a support system, so you have people taking care of you while you take care of your child.
“It can be a long road, but you have to hang in there,” said Cameo, a mentor with the Parents Offering Parent Support (POPS) program at Children’s Mercy. “There really is light at the end of the tunnel. Transplant is [a treatment,] not a cure, but it will really help. There’s hope.”
The friends Morea grew up with know about her transplant, encourage her to stay hydrated and have been checking the organ donor box when they get their driver’s licenses. But many of her peers have no idea.
“They’re just like, ‘What do you mean you only have one [kidney]?’” said Morea. “I explain I had a disease. I had to get them taken out and get a new one. And then they kind of just accept that.”
And why wouldn’t they? Morea’s kidney status hasn’t held her back as a teenager. But it has made her curious about nursing as a career. Next year, she’s taking an Intro to Health Science Careers class that will help her explore that possible pathway. But before then, summer!
“Tryouts are coming up, and I’m really looking forward to continuing with all my dance next season,” said Morea. “And I’m very much looking forward to summer and freedom and being able to hang out with my friends!”