Wide World of Vaccines
July 2021
Two mRNA Vaccine Doses Needed for Delta and Emerging Gamma Virus; Myo/pericarditis Data

Column Editor: Christopher Harrison, MD | Professor of Pediatrics, UMKC School of Medicine | Clinical Professor of Pediatrics, University of Kansas School of Medicine
The pandemic news is mixed.
The good news is fewer hospitalizations (~18,000/day) and deaths (~200/day) despite the total number of deaths reported as of July 8, 2021 being 605,426. The bad news is slow vaccine uptake has led to the virus staging a comeback (70% increase nationally in cases since June 21, 2021) mostly in low-vaccine-uptake areas and due mostly (85%) to the Delta variant (e.g., 196% increase in Cherokee County, Kan.).
mRNA vaccines (Pfizer and Moderna) are working in the U.S., with >90% protection against the original and against the Alpha (U.K.) viruses. Against the Delta virus (started in India), two-dose schedules remain highly protective (mid-90% against severe illness, hospitalizations and death). Breakthrough infections do occur after intense exposures but are nearly uniformly asymptomatic or minimally symptomatic.
But if you did not get the second dose, protection against Delta virus drops like a rock to ~30% against symptomatic disease. Protection against the Gamma virus (started in Brazil) is less clear. mRNA vaccine-induced antibody neutralizes both viruses in vitro but needs higher titers to do so. Preliminary data suggest that two mRNA vaccine doses seem to provide mid-80% protection against hospitalization and death against the Gamma virus. It is unclear how much protection that one dose provides. Of note, the Johnson & Johnson vaccine (a one-dose regimen) was recently reported to induce antibody for up to eight months and neutralizes the original, the Alpha, the Delta and the Gamma viruses,1 and clinical disease due to breakthroughs does not seem more frequent with the Delta virus.
To focus on how well full vaccine schedules protect, 98% of COVID-19 deaths and >95% of hospitalizations are now in unvaccinated persons.
But there are ongoing concerns.
- The increasing case numbers are due to the emerging variants (Delta and Gamma viruses – 321,000 new cases/day nationally with 85% being Delta and 5-10% being Gamma). Four Missouri counties are in the top 10 nationally for increasing case rates (Joplin, Taney, Polk and Newton Counties).
- There is lagging vaccine uptake of first and second doses particularly in teens and young adults (plateauing and not yet 70% for >18-year-olds).
- Rare post-mRNA vaccine myo/pericarditis (mostly in late teens and young adult males).
Every state now has the Delta virus. The Gamma virus is mostly in Washington state with a few other coastal pockets. Why is that important? Because the Delta virus is two to four times more transmissible than the Alpha virus, even in mild cases, likely due to the much larger amounts of the Delta virus produced in the airway during infections. Luckily, the Delta virus does not seem to cause more hospitalizations/deaths than the Alpha virus, but hospitalizations are now occurring in mostly younger populations, e.g., teens through 30-year-olds.
Also, the Gamma virus is not only nearly as transmissible as the Delta, but the Gamma variant is also more deadly. And don’t look now, but India health authorities are reporting a new Gamma-sub-variant that looks even more transmissible with stronger binding to lung cells than the parent Gamma virus. These new variants bode poorly for the unvaccinated and we are seeing major surges in regions with low vaccination rates.
How bad will it be? Cases, hospitalizations and deaths are now increasing disproportionately in rural areas (areas with lowest vaccine uptake).2,3 As far as test positivity rates and percent increase in cases, Kansas and Missouri are among the worst for both. Figures 1 and 2. And unfortunately, increased case rates in areas with lower-than-average vaccination rates (e.g., Missouri and Kansas) have paralleled increases in death rates. Figure 3. Missouri and Kansas have death rates that are 50% and 100% higher than the national average.4 It seems clear we need to continue to advocate strongly for the mRNA COVID-19 vaccines available in the U.S.
Caveat: If an unvaccinated person has not yet had COVID-19 infection, they are almost assuredly going to get one variant or another before next summer. And we should also expect the unvaccinated who are mistakenly relying on immunity from infection with the original virus to also be vulnerable to the Delta and Gamma variants.
Myopericarditis. How concerned should we be and how do we counsel families regarding vaccine-associated myo/pericarditis? The data, as with all things related to SARS-CoV-2, are preliminary and the analyses so far are not truly population-based. So, stating a definite risk is not possible. That said, the data deserve our attention. Certain aspects seem established. Acute onset of chest pain three to five days post-vaccine dosing, mostly after second mRNA doses, seems the best sign that a person needs evaluation. This timeline in reported cases suggests an immune-mediated pathogenesis.5 In the Vaccine Adverse Effects Reporting System (VAERS), data presented to the Advisory Committee on Immunization Practices (ACIP) in late June,6 there were 128 myo/pericarditis reports in 12-17-year-old males from 2,019,871 doses (0.00627%) and 19 reports in 12-17-year-old females from 2,189,726 doses (0.00087%). Myo/pericarditis is usually very rare in pre-teens and teens, so despite the post-vaccine rates being extremely small, they are 30 to 100 times the background expected rate for males and 10 to 20 times that in females. Other data suggest that older males and females have rates mostly lower than young females. So, risk is definitely highest, albeit very small, in young males.
But what is the rate of myocardial injury in teens/young adults who get COVID-19 infections? Precise data are also not available for COVID-19 myo/pericarditis, but estimated rates are between 0.8% and 2.3% for non- or mildly symptomatic young males.7,8 In an expert report by M. Imazio, MD, released by the American College of Cardiology on Feb. 5 2021, about COVID-19 possibly causing myocarditis, rates were estimated at 8% to 22% in hospitalized adults, up to 22% if needing ICU, and up to 59% in fatal cases (used elevation of cardiac troponin I >99th percentile upper reference limit as criterion). The pre-teen and teen myo/pericarditis rates post-vaccine are higher than background (particularly in males), but nowhere near the estimated risk of myocardial injury seen in adults with even mild COVID-19 infection.
Bottom line: Two doses of mRNA vaccine is the best protection against COVID-19 variant disease and the small risk of post-vaccine myo/pericarditis (from which recovery is almost assured within one week) should not deter families from having their 12-18-year-old children immunized. As the vaccine is approved for younger children, expect a lower dose aimed at reducing reactogenicity, so hopefully the rare post-vaccine myo/pericarditis will be even lower in younger vaccinees.
Figure 1. U.S. COVID-19 test positivity rate for week ending July 5, 2021. Missouri and Kansas were among the worst five states.
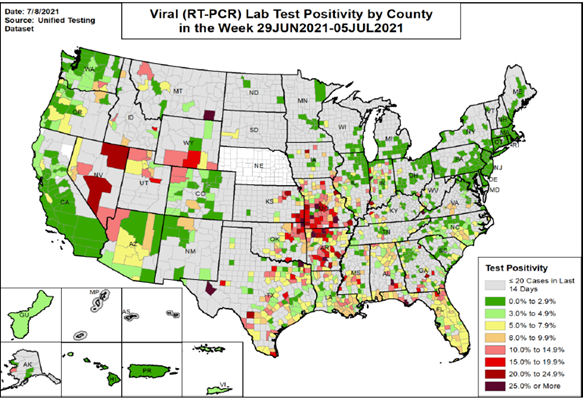
Source: https://healthdata.gov/Health/COVID-19-Community-Profile-Report/gqxm-d9w9
Figure 2. U.S. COVID-19 rate of change for new cases for week ending July 7, 2021.
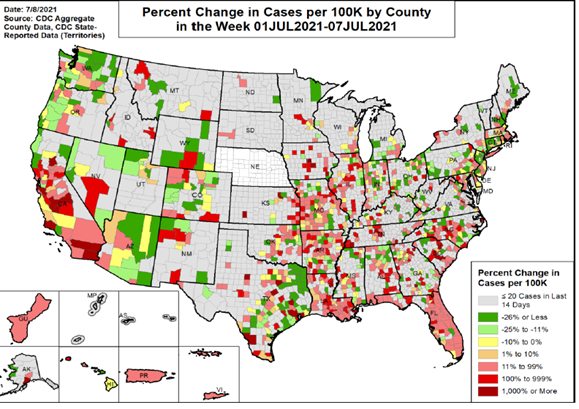
Source: https://healthdata.gov/Health/COVID-19-Community-Profile-Report/gqxm-d9w9
Figure 3. Change in deaths/100,000 population for week ending July 7, 2021, by county. Average change for whole U.S. was down 25% compared to increases of 25% or more in 21 Missouri and seven Kansas counties.
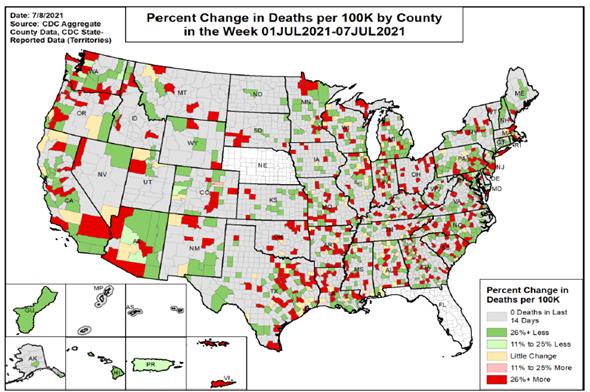
Source: https://healthdata.gov/Health/COVID-19-Community-Profile-Report/gqxm-d9w9
References:
- Jongeneelen M, et al. Ad26.COV2.S elicited neutralizing activity against Delta and other SARS-CoV-2 variants of concern. bioRxiv 2021.07.01.450707; doi: https://doi.org/10.1101/2021.07.01.450707.
- https://www.nytimes.com/interactive/2021/us/covid-cases.html.
- https://vaccine-hesitancy.healthdata.org/.
- https://covid.cdc.gov/covid-data-tracker/#cases_deathsper100klast7days.
- Stone CA Jr, et al. Immune-mediated adverse reactions to vaccines. Br J Clin Pharmacol. 2019;85(12):2694-2706.
- Gargano J et al. Use of mRNA COVID-19 vaccine after reports of myocarditis among vaccine recipients: Update from the Advisory Committee on Immunization Practices — United States, June 2021 MMWR July 9, 2021 70(27) 977-982.
- Martinez, MW et al. Prevalence of inflammatory heart disease among professional athletes with prior COVID-19 infection who received systematic return-to-play. Cardiac Screening. JAMA Cardiol. doi:10.1001/jamacardio.2021.0565 Published online March 4, 2021.
- Daniels, CJ et al. Prevalence of clinical and subclinical myocarditis in competitive athletes with recent SARS-CoV-2 infection results from the Big Ten COVID-19 Cardiac Registry. JAMA Cardiol. doi:10.1001/jamacardio.2021.2065 Published online May 27, 2021.