Wide World of Vaccines
April 2021
Previously Infected Patients Need SARS-CoV-2 Vaccine: mRNA Vaccines Induce More Consistent Neutralizing Antibodies to Standard and Variant Virus Than Prior Infection

Author: Christopher Harrison, MD | Professor of Pediatrics, UMKC School of Medicine | Clinical Professor of Pediatrics, University of Kansas School of Medicine
Do previously SARS-CoV-2 infected patients need vaccine – and do mRNA vaccines induce more neutralizing antibodies to standard and variant virus than prior infection?
Previous data show that neutralizing antibody (NtAb) to SARS-CoV-2 is key to protecting against disease.1 Other data have also shown variable responses after infection and that infection-induced neutralizing antibody may wane quickly (as little as three months) in some patients.2 The data on the persistence of NtAb after the vaccines continues to evolve, but NtAb appears to persist for at least six months. It may last longer, but data are only available for six months because we have only been giving the vaccine for six months, even to experimental subjects. Now two studies add details and more clarity on NtAb after infection3 and the effect of mRNA vaccines on NtAb in people who have recovered from infection, versus those who received vaccine without prior infection.4
These data could impact recommendations on who should receive vaccine, how many doses and at what intervals. Also, these data point out the folly of voluntarily getting infected as an easy way to get protection without taking a vaccine in younger people (<40 years old). Note: The new variants are in all states and are causing severe disease more often in younger people. This is also a reason to not be cavalier about unnecessary exposures.
Investigators from Singapore analyzed initial cytokines/chemokines during infection plus peak antibody levels, and waning of NtAb to a non-variant SARS-CoV-2 virus over six months after infection in nearly 300 patients. They also correlated NtAb with patients’ initial clinical disease severity.3 They found five different groups in regard to NtAb development/persistence:
- 12% poor responders who never had detectable NtAbs, although all in this group produced non-neutralizing antibodies (non-neutralizing antibodies do not appear to be protective).
- 27% rapid waners who had NtAbs in the first month post-infection, rapidly waned by about 40 days, and sero-reverted (lost NtAb) by six months post-infection.
- 29% slow waners whose NtAb persisted at six months but dropped to minimal levels at three to six months.
- 32% persistent responders whose NtAbs decreased very little after six months.
- 2% ongoing responders whose NtAb unexpectedly continually increased over three to six months.
Further, NtAb loss or severe titer drops by six months were associated with asymptomatic/non-severe infections (and only temporary, if any, production of proinflammatory cytokines/chemokines). Interestingly, these authors developed a machine learning algorithm to predict NtAb persistence beyond six months (up to 30 years). The predictive algorithm was applied to the patients and categorized study subjects into three groups (Figure 1 - a rapidly waning group, a slowly waning group, and a persistent group). This also mostly correlated to asymptomatic/mild, modest and severe initial severity of disease, respectively.
Bottom line: Do not count on natural infection to consistently produce persistent neutralizing antibody, even if against the original SARS-CoV-2 strain (as many as 40% may be vulnerable to reinfection by six months). And the milder the COVID-19 disease appears, the less likely it is to protect from reinfection at or beyond six months (similar to varicella). To date, it does appear that reinfections with non-variant strains are generally not severe and protection seems good against the UK variant. However, protection against the Brazilian or South African variants (unclear about the California variant at this time) may only be ~40% at max, given that neutralizing antibody induced by the non-variant strains is only ~30 to 40% active against the variants. These data highlight the ongoing need for social mitigation and raise concerns as to whether older children or young adults who have had mild or asymptomatic infections may become vectors in the months to come.
Are vaccines more protective either in previously infected or previously uninfected populations; and if so, how many doses are needed? Data from the state of Washington in several dozen patients address the capacity of sera from vaccinated convalescent patients and from infection-naïve vaccinees to neutralize the Wuhan-Hu-1 (original virus) and South African B.1.351 variant.4
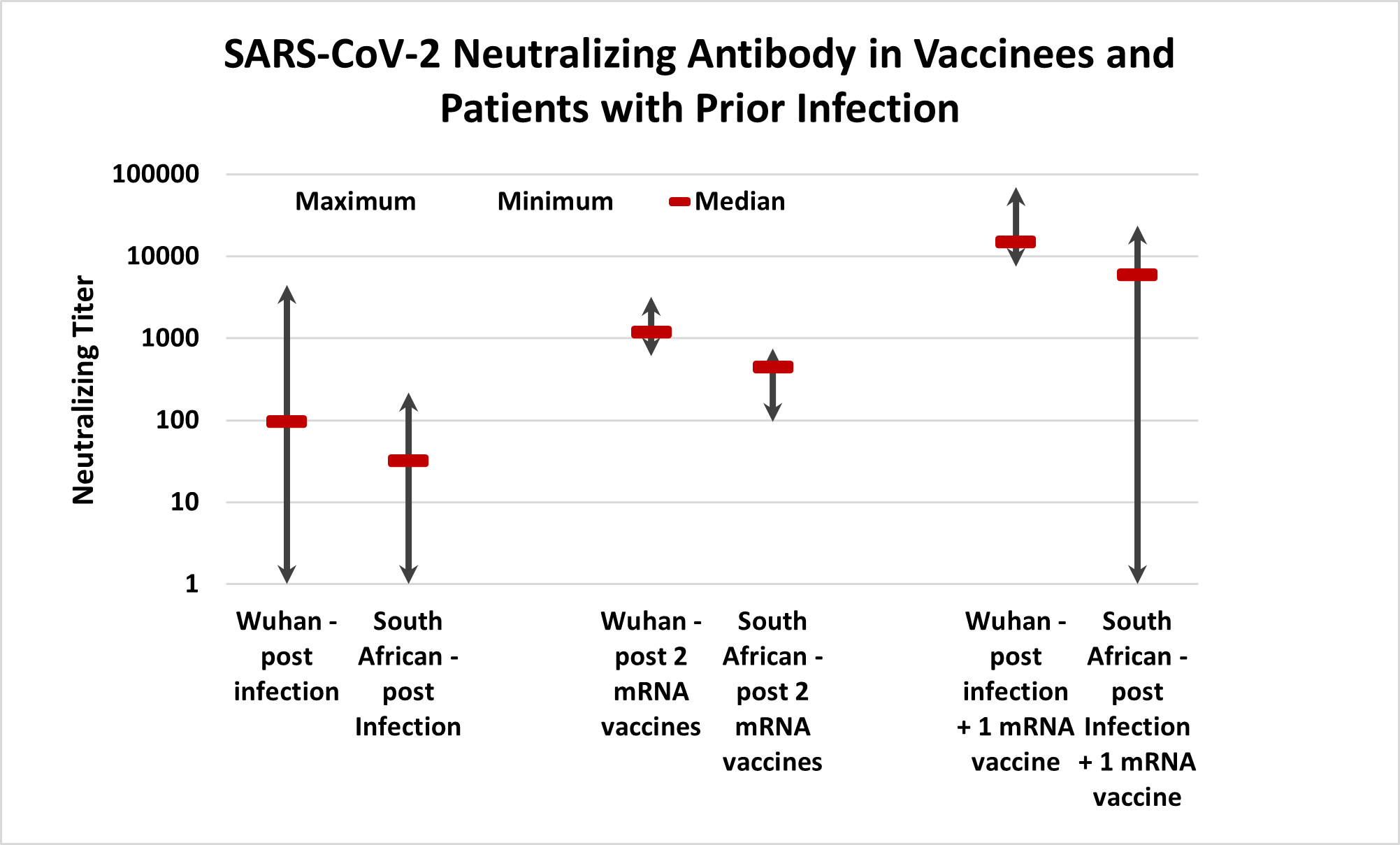
In this study, post-infection sera (approximately six months post-infection) were able to neutralize Wuhan-Hu-1 (80%) and B.1.351 (33%) with median titers ~1:100 and ~1:64, respectively. In sera from these same patients two to three weeks post one mRNA dose, NtAb titers boosted several hundred-fold to both Wuhan-Hu-1 and B.1.351. (Figure 2) This is great news, but note that NtAb was still undetectable in 13% to B.1.351 post-vaccine, so it’s not a sure thing for the variant even after one vaccine dose.
Sera from previously non-infected vaccinees had no NtAb pre-vaccine as expected, but three to four weeks after their second doses, all had NtAb (lowest ~1:800 for Wuhan-Hu-1 and ~1:100 for B.1.351) and median titers were above 1,000 for Wuhan-Hu-1 and ~750 for B.1.351. (Figure 2)
Unlike previously infected patients, getting a dose of vaccine six months post-infection, previously non-infected vaccinees did not get a boost from the second dose three to four weeks after the first dose. So, it appears the second dose soon after the first dose of mRNA vaccines is not a boosting dose, and perhaps a better (boosting) response would be more likely with a delay between the first and second dose.
However, before we call for delayed second doses, we must remember that the number of patients was small in the latter study and needs confirmation. The study does provide a strong suggestion that previously infected patients need to get at least one vaccine dose with the caveat that they may not get an adequate response or boost in NtAb against the new variants. The lack of NtAb after one mRNA dose in previously infected patients means that they could need either a second mRNA dose or a variant-specific vaccine. Studies are underway concerning the second dose approach, and phase 1 studies have begun on variant-specific vaccines. So as usual with SARS-CoV-2, stay tuned.
Figure 1. Prediction of neutralizing antibody (NtAb) based on titers in the first six weeks after infection.
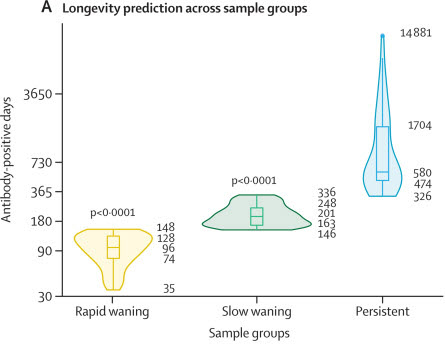
Adapted from (3). Note that disease severity was mostly minimal in rapid waners, mostly modest in slow waners, and mostly severe in persistent responders. The numbers alongside the graph figures are the number of days that NtAb is predicted to persist. Figure licensed under a Creative Commons Attribution 4.0 International (CC BY 4.0) license, which permits unrestricted use, distribution, and reproduction in any medium, provided the original work is properly cited.
Figure 2. Comparison of responses to mRNA vaccine in previously SARS-CoV-2 infected patients (one dose) and previously uninfected vaccinees (two doses) three to four weeks after last vaccine dose. Adapted from (4).
References:
- Addetia A, Crawford KH, Dingens A, et al. Neutralizing antibodies correlate with protection from SARS-CoV-2 in humans during a fishery vessel outbreak with high attack rate. Preprint. medRxiv. 2020;2020.08.13.20173161. Published 2020 Aug 14. doi:10.1101/2020.08.13.20173161.
- Robbiani DF, et al. Convergent antibody responses to SARS-CoV-2 in convalescent individuals. Nature. 2020;584:437–442. doi: 10.1038/s41586-020-2456-9.
- Wan Ni Chia*, et al. Dynamics of SARS-CoV-2 neutralising antibody responses and duration of immunity: a longitudinal study. Lancet Microbe 2021. Published Online. March 23, 2021. https://doi.org/10.1016/S2666-5247(21)00025-2.
- Stamatatos, et al. mRNA vaccination boosts cross-variant neutralizing antibodies elicited by SARS-CoV-2 infection. Science. 10.1126/science.abg9175 (2021). published online March 25, 2021.