What's the Diagnosis?
March 2021
Visual Diagnosis
Column Author/Editor: Joe Julian, MD, MPHTM, FAAP | Hospitalist, Internal Medicine - Pediatrics | Assistant Professor, Internal Medicine and Pediatrics, UMKC School of Medicine
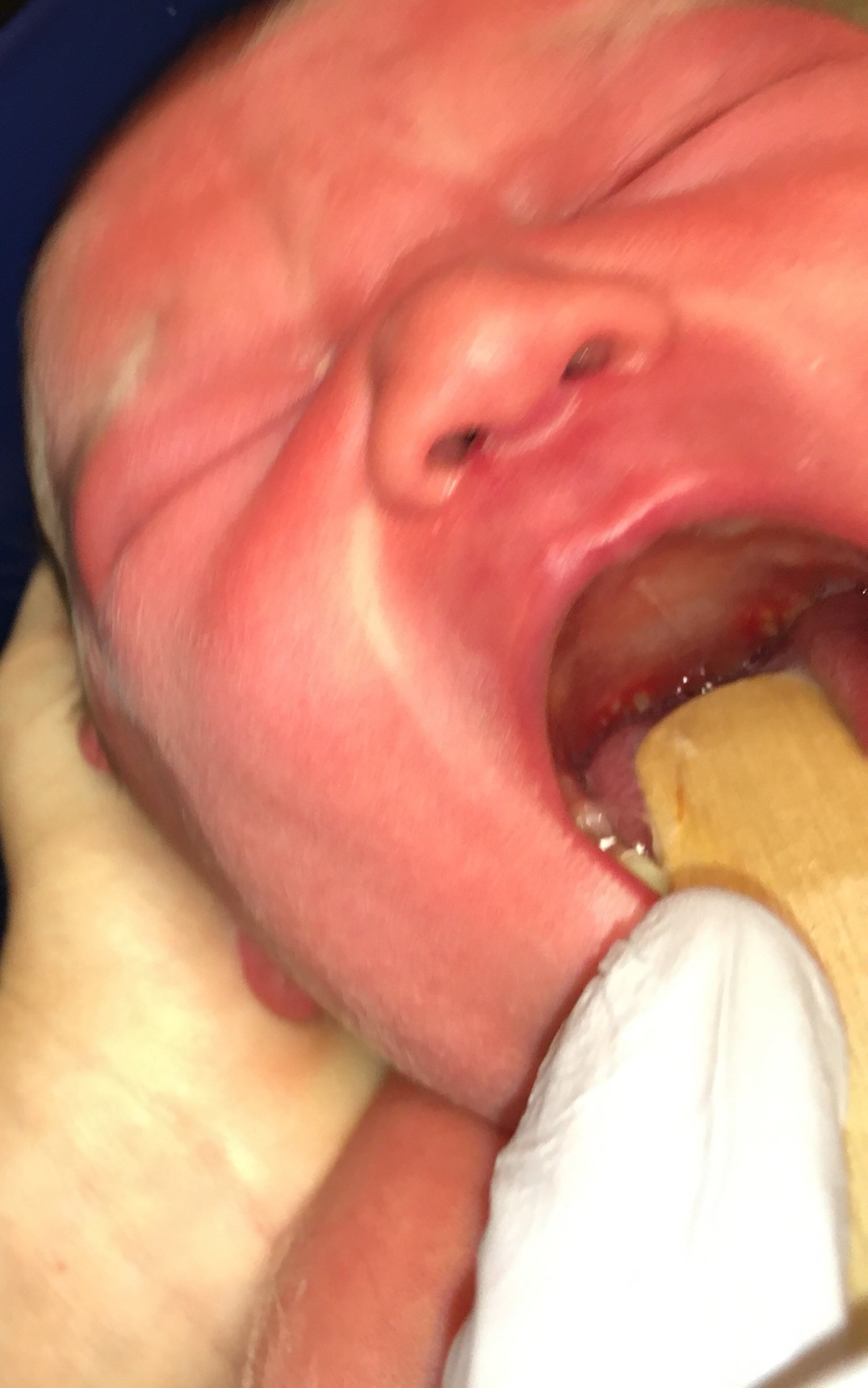
A 4-day-old female is seen in a primary care office to establish care. While examining the palate, the patient’s pediatrician incidentally notes vesicles on the oropharynx concerning for herpes simplex virus (HSV). Direct admission is requested for further evaluation.
The patient was born via spontaneous vaginal delivery at term without any complications during pregnancy or during nursery stay. There are no fevers, rashes or irritability. She is exclusively breastfed without difficulties. The mother has a history of a primary HSV outbreak five years ago, but has had no outbreaks since (including around time of delivery). The patient has only been in contact with her parents and older sister. None of these family members have any active lesions and there are no sick contacts.
Vitals signs are unremarkable and there is no fever. She is non-toxic in appearance. There are several symmetric vesicular lesions with erythematous bases surrounding the uvula. There are no lesions on the remainder of the oral mucosa. There is no scleral injection or conjunctivitis. There is some erythema toxicum present on the torso, but there are no vesicles on the palms, soles, buttocks or groin. The cardiopulmonary and neurologic examination are normal.
CBC is notable for a WBC count of 17K (upper limit of normal for age 21K) with an unremarkable differential. Empiric acyclovir IV is started. Skin, eye, mucous membrane and oropharyngeal lesion samples are obtained for HSV PCR. A lumbar puncture is performed (unremarkable with 4 RBCs, 2 WBCs) and CSF is also sent for HSV PCR. All PCR testing returns negative for HSV.
What is the next best step in management for this patient?
A. Continue acyclovir IV
B. Investigate for non-accidental trauma
C. Consult lactation specialist
D. Prescribe oral nystatin
Answer: C. Consult lactation specialist
This patient’s vesicles are consistent with pterygoid ulcers (Bednar aphthae). This is a benign mucosal finding that is usually found incidentally. It is infrequently described in the literature despite its prevalence (~15% of all newborn infants). The ulcers start as hyperemic areas, progress to small vesicles, and ultimately coalesce prior to healing. They were initially thought to be caused by trauma during feeding (specifically bottle but can occur with breastfeeding). There is some speculation that they are immunologic in nature and related to antigens in the breast milk. The treatment is to avoid horizontal feeding positions and, if applicable, use an orthodontic nipple with a larger opening. A lactation specialist can assist with positions to reduce trauma on the uvula. These ulcers are ultimately self-limiting. In the absence of other findings, there is no association with non-accidental trauma.
While the individual lesions may have a herpetic appearance, all the lesions were negative by PCR and there is no additional evidence of skin-eye-mucous membrane HSV infection. Infectious etiologies such as HSV, hand-foot-mouth disease, and candidiasis usually have distribution throughout the oral mucosa (not focal as described with pterygoid ulcers). Nystatin and other antimicrobial therapies are not warranted.
There is a scarcity of literature on this topic and diagnostic evaluation for this condition is difficult. One must balance the potential for a missed HSV infection despite a well-appearing infant vs. performing a lumbar puncture for a benign condition. Commentary on this topic is varied as well with some recommending a full diagnostic workup for HSV, while others recommend outpatient management and watchful waiting if HSV PCR testing of the vesicles can be completed in a timely fashion. Shared decision-making with parents is paramount.
References:
- Hartsell A, Nagappan S. Posterior oropharyngeal ulcers in a neonate. NeoReviews. 2012; 13(11): e687-e689.
- Johng SS, Gribben V, Laves E. An infant with ulcerative lesions of the posterior oropharynx. Pediatr Rev. 2020; 41(8): e31-e33.
- Nebgen S, et al. Bednar’s aphthae in neonates: incidence and associated factors. Neonatology. 2010; 98(2): 208-211.
