What's the Diagnosis?
July 2022
Visual Diagnosis

Author: Phil Jurasinski, DO, MPH, MSN | Internal Medicine – Pediatrics Resident, PGY-2
Column Editor: Joe Julian, MD, MPHTM, FAAP | Hospitalist, Internal Medicine – Pediatrics | Clinical Associate Professor, Internal Medicine and Pediatrics, UMKC School of Medicine
A 5-month-old male with a pertinent history of atopic dermatitis presents to the emergency department for progressive rash. His symptoms started three days ago. He developed red bumps primarily on his left arm and chest which subsequently spread over the next two days. Blisters started forming on his face, and the other lesions started to leak clear fluid. The patient’s mother feels that this looks different from his usual atopic dermatitis and sought care at the emergency department.
Maternal history is notable for COVID-19 during the third trimester. The family denies any history of herpes simplex virus (HSV) during pregnancy. He was born vaginally at 40 weeks of gestation. He did require a NICU stay for hyperbilirubinemia due to blood type incompatibility, but his mother does not know any further details. He attends child care and the family believes that he possibly may have been exposed to an infection there.
Previous medications include intermittent use of triamcinolone, hydrocortisone, A&D ointment and mupirocin.
Vital Signs and Physical Exam
- Vital signs: Febrile on presentation but otherwise within age-appropriate limits.
- General: Awake, alert, in no distress.
- Eyes: No conjunctival injection or scleral icterus.
- Lymph: No lymphadenopathy.
- Ear/Nose/Throat: Mucous membranes moist, no lesions, no tonsillar exudates and no nasal discharge.
- Skin: Erythematous papulovesicular rash predominantly on the left side of the face, trunk, left arm and left upper thigh. Lesions of the left cheek are noticeably crusted. Sparse erythematous papular lesions on back and right lower extremity as well as right arm. Soles and mouth are spared. (see images below)
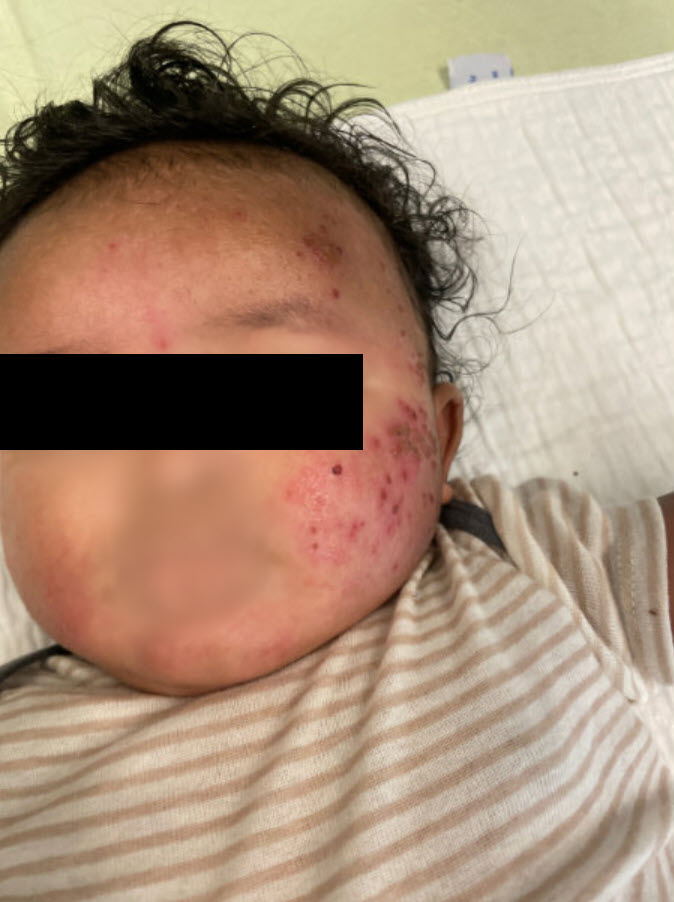
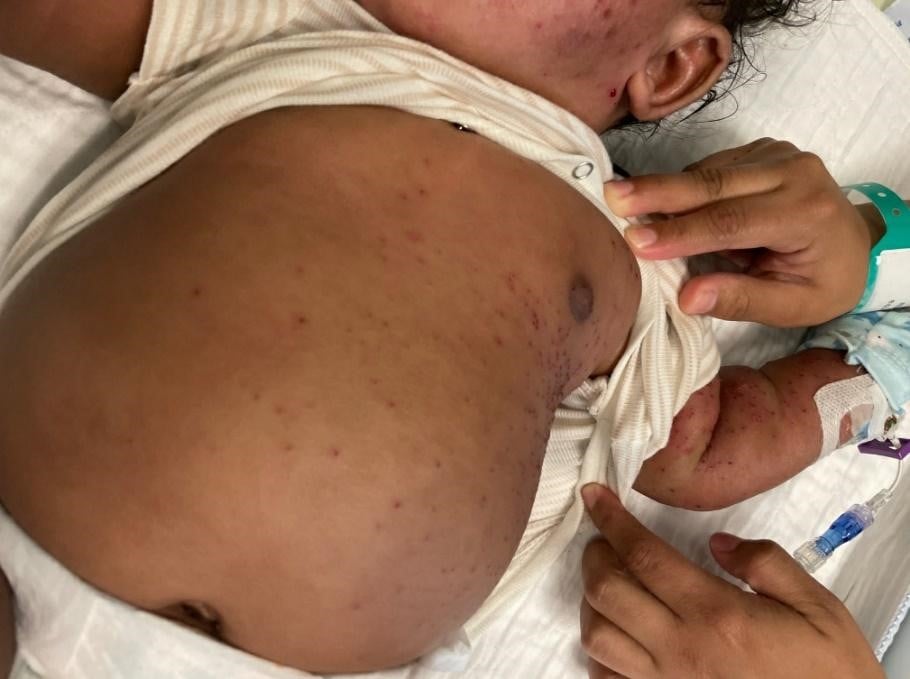
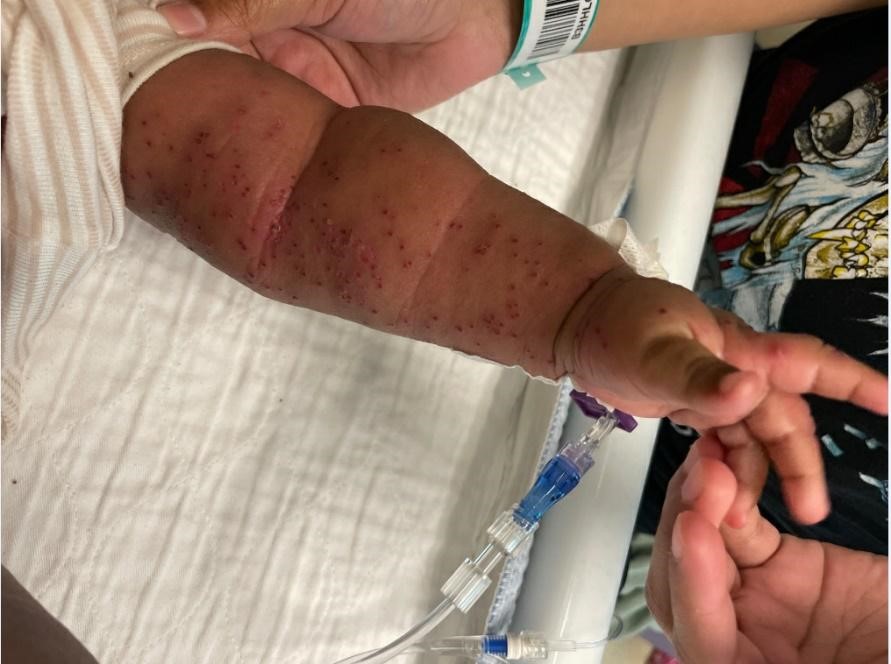
Questions
1) What is the most likely diagnosis for this patient?
A. Impetigo
B. Eczema herpeticum (EH)
C. Molluscum contagiosum
D. Primary varicella infection
E. Acute generalized exanthematous pustulosis (AGEP)
Answer: B. Eczema herpeticum (EH)
Also known as Kaposi varicelliform eruption, eczema herpeticum presents as non-grouped vesicular lesions and pustules on erythematous lesions that lead to erosions in two to seven days.1 While AGEP can also present with a pustular rash, there is typically exposure to a precipitating drug and a more diffuse distribution. Primary varicella can have pustular and crusting lesions as noted above, but these typically appear in groups that are in different stages of development. Molluscum contagiosum causes umbilicated papular lesions and fever is not present. Impetigo can have pustular lesions, but the “golden crusting” is not seen in EH.
Although EH is diagnosed clinically, there is a lack of clinical diagnostic criteria to diagnose the infection. Hallmarks include non-grouped vesicular eruptions, vesicles and erosions focused on areas of atopic dermatitis, fever, malaise, and EH episodes in the patient history.1 Diagnosis is confirmed by HSV polymerase chain reaction (PCR).
Twenty percent of EH patients can present with a medical history of HSV. EH is associated with atopic dermatitis but also can be associated with Darier disease in adult patients.1 More severe forms of EH are associated with high scores on the Eczema Severity Index and a higher amount of body surface area involvement.2 Patients are more likely to have food and environmental allergies, asthma, early onset of atopic dermatitis before age 5, and history of Staphylococcus aureus and molluscum contagiosum infections.1,3 Hospitalization for EH is also noted more likely to occur in non-White ethnicities and in metropolitan areas.2
Treatment of atopic dermatitis with corticosteroids does not necessarily lead to a higher incidence of EH. Recurrences of EH have been noted to be slightly higher in winter and spring months.1 The clinical course can progress to a bacterial superinfection, most notably with streptococci and staphylococci.1
2) What is the best course of treatment for this condition?
A. Oral valacyclovir
B. Intravenous acyclovir
C. Intravenous foscarnet
D. Oral prednisolone
Answer: B. Intravenous acyclovir
Acyclovir is considered the mainline treatment for first presentations of EH as seen in this patient.1 This treatment course is also recommended for patients who are immunocompromised. In immunocompetent patients, recurrent flares of EH are often less severe and may be treated with valacyclovir for seven days.1 Foscarnet is reserved for acyclovir-resistant strains in EH and may need to be considered for immunosuppressed patients.1 Systemic glucocorticoids are not recommended for treatment of EH and, when combined with JAK 1 and 2 inhibitors, increase the incidence of EH.1 Topical treatments that target active eczema and secondary infection are recommended, as is adequate analgesia.
Clinical Course
The emergency department contacted dermatology and infectious diseases, which recommended HSV PCR of the lesions. The patient was discharged home via shared decision-making and prescribed oral acyclovir four times daily. The patient’s lesions continued to spread, and his fevers persisted. His family returned to the emergency department the next day, and he was subsequently admitted to the hospital. HSV PCR of his lesions resulted as positive by the time of admission. Based on the spread of lesions despite being on oral acyclovir, he was started on IV acyclovir.
The patient remained afebrile in stable condition. Infectious disease, dermatology and ophthalmology were all consulted for his lesions. Infectious disease recommended a seven- to 10-day course of oral antivirals. Dermatology recommended a combination of Domeboro soaks, petroleum jelly and topical steroids. Antibiotics were not given as there was no concern for bacterial superinfection. Ophthalmology was consulted due to lesions located close to his eye; they evaluated him with no concerns of ocular involvement. He was discharged three days after admission. He followed up in the dermatology clinic eight days later where he was found to have improved lesions and was advised to continue the soaks while the lesions were healing. He had another appointment with dermatology one month after admission where they increased the potency of his triamcinolone and hydrocortisone cream, recommended bleach baths a few times a week, and advised him to stop the Domeboro soaks as his flare of EH had resolved at that time.
References:
- Traidl S, Roesner L, Zeitvogel J, Werfel T. Eczema herpeticum in atopic dermatitis. Allergy. 2021;76(10):3017-3027. https://onlinelibrary.wiley.com/doi/pdf/10.1111/all.14853
- Hsu DY, Shinkai K, Silverberg JI. Epidemiology of eczema herpeticum in hospitalized U.S. children: analysis of a nationwide cohort. J Invest Dermatol. 138(2):265-272. https://www.sciencedirect.com/science/article/pii/S0022202X17329470
- Xiao A, Tsuchiya A. Eczema herpeticum. Updated August 2021. In: StatPearls [Internet]. StatPearls Publishing; January 2022.
