What's the Diagnosis?
August 2021
Visual Diagnosis
Column Editor: Joe Julian, MD, MPHTM, FAAP | Hospitalist, Internal Medicine - Pediatrics | Assistant Professor, Internal Medicine and Pediatrics, UMKC School of Medicine
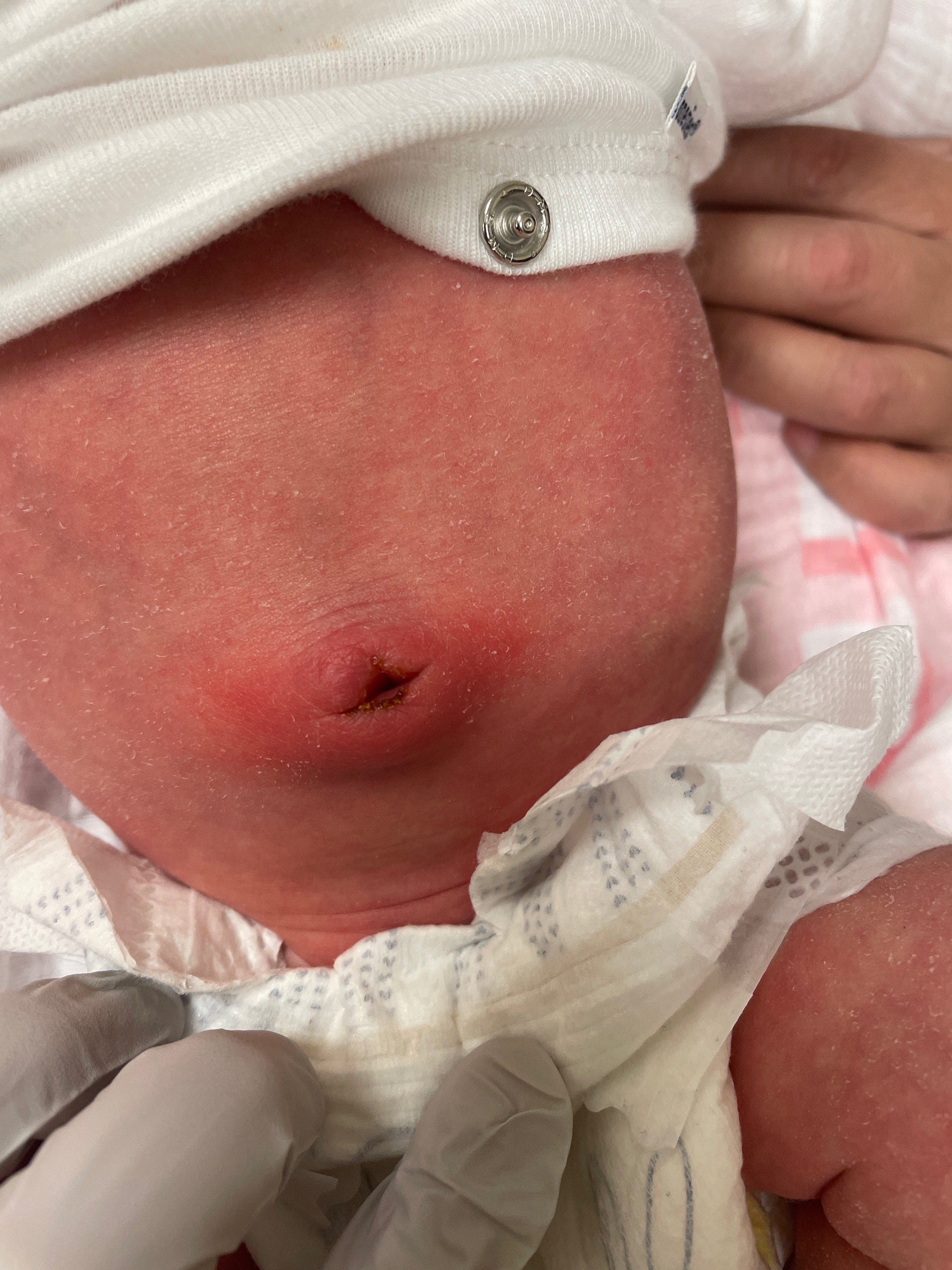
A 2-week-old female is seen in the Emergency Department for redness around her umbilicus. Her umbilical cord stump fell off approximately one week ago. There were no concerns until her parents noticed redness around her umbilicus 24 hours ago. There is associated swelling with yellow drainage and crusting. There is no associated fever, respiratory distress, decrease in feeding or urine output, and no additional skin changes. The redness continued to spread over the past day and medical attention was sought. Admission was requested for further management.
The patient was born at 35 weeks’ gestational age due to maternal pre-eclampsia. The mother received adequate intrapartum treatment for Group B Streptococcus. Nursery course was unremarkable, and she is gaining weight appropriately.
Vital signs are unremarkable and there is no fever. She is non-toxic in appearance. There is erythema and edema of the umbilicus with periumbilical involvement. There is some scant crusting and discharge inside the umbilicus. No necrotic areas or crepitus are present. There is no jaundice, and the remainder of the examination is unremarkable.
CBC is notable for a WBC count of 8K (upper limit of normal for age 19.5K; differential 1% immature cells and 39% neutrophils) and mild platelet elevation to 491 (upper limit of normal for age 450). C-reactive protein (0.7 mg/dL) and ESR (3 mm/hr) are both within normal ranges. Cultures of blood and umbilical drainage are obtained and pending. Gram stain of umbilical drainage is notable for Gram positive cocci in clusters, rare white blood cells, and a few squamous epithelial cells.
What is the best antimicrobial option for this patient?
A. No antibiotics, local wound care only
B. Intravenous vancomycin + piperacillin-tazobactam
C. Intravenous clindamycin + ceftazidime
D. Oral amoxicillin
Answer: C. Intravenous clindamycin + ceftazidime
The selection of antimicrobial therapy for omphalitis varies depending upon the geographic setting (developing versus developed countries) and the illness severity (presence of sepsis or necrotizing infection). In this setting, the most common pathogen is Staphylococcus aureus followed by group A and B Streptococcus, and non-pseudomonal Gram negative rods (such as Escherichia coli and Klebsiella species). Additional pathogens can include Clostridium, Bacteroides, and Pseudomonas species.
Local wound care is insufficient. Oral amoxicillin does not provide staphylococcal coverage and omphalitis necessitates parenteral therapy. This patient does not have evidence of a necrotizing infection and is not ill-appearing which makes vancomycin + piperacillin-tazobactam an unnecessarily broad choice. Infants who are severely ill or already in the intensive care setting are probably more appropriate for antimicrobial therapy targeted toward Pseudomonas aeruginosa (e.g., cefepime, piperacillin-tazobactam).
Intravenous clindamycin + ceftazidime is the most appropriate antimicrobial choice as it will provide coverage for the most common organisms noted above. The substitution of gentamicin for ceftazidime would also provide similar coverage. There is no absolutely “correct” regimen as the literature is quite varied in terms of microbiology as geographic location and resource availability play a significant role in this.
This patient was started on clindamycin and cefepime. The culture of the umbilical drainage grew out Methicillin-susceptible Staphylococcus aureus (MSSA) and diphtheroid species. The patient was switched to ampicillin-sulbactam IV which was continued until the erythema was almost completely resolved. She was transitioned to oral amoxicillin-clavulanate at discharge to complete a 10-day course of antibiotics per the recommendation of the infectious diseases consultant. Of note, the patient’s blood culture grew out Staphylococcus epidermidis which was deemed to be a contaminant. Lumbar puncture was considered prior to the identification of the blood culture pathogen but was ultimately held as true bacteremia was not present. Ultrasound imaging did not show any evidence of omphalomesenteric remnants.
References:
- Hemananda M, Sardesai T, and Sardesai S. Disorders of the umbilical cord. Pediatrics in Review. 2018; 39(7): 332-341.
- Sawardekar K. Changing spectrum of neonatal omphalitis. Pediatr Infect Dis J. 2004; 23(1): 22-6.
- Stewart D and Benitz W. American Academy of Pediatrics: Committee on Fetus and Newborn. Umbilical cord care in the newborn infant. Pediatrics. 2016; 138(3): e1-7.
- Zahouani T, Recinos A, and Mota J. Clinical image: omphalitis. Annals of Clinical and Laboratory Research. 2016; 4(4):135.
