Outbreaks, Alerts and Hot Topics
September 2022
Poliomyelitis in the United States: 2022

Author: Chris Day, MD| Pediatric Infectious Diseases | Director, Transplant Infectious Diseases & Travel Medicine | Assistant Professor of Pediatrics, UMKC School of Medicine
Column Editor: Angela Myers, MD, MPH | Director, Division of Infectious Diseases | Professor of Pediatrics, UMKC School of Medicine | Medical Editor, The Link Newsletter
Earlier this summer, an unvaccinated young adult in Rockland County, New York, was hospitalized with acute flaccid weakness in his lower extremities. The New York State Department of Health notified the Centers for Disease Control and Prevention (CDC) that a vaccine-derived strain of poliovirus (VDPV) type 2 was detected from the patient’s stool. The patient had not traveled internationally during the possible period of exposure but had attended a large gathering. Further epidemiologic investigation was done including testing of local wastewater, which included samples available from COVID-19 surveillance that predated the patient becoming ill. Vaccine-derived poliovirus type 2 that was genetically linked to the patient’s virus was found in 21 of the 260 wastewater samples from Rockland County and neighboring Orange County. This case represents only the second time that a community transmission of any poliovirus had been documented in the United States since 1979.1
Understanding polioviruses
The polioviruses are made up of three distinct serotypes (types 1, 2 and 3), which are closely related to other enteroviruses. Humans serve as the only natural hosts. Most infections with polioviruses are asymptomatic or only mildly symptomatic with aseptic meningitis occurring in 4%-8% of all infected children.2 Approximately 0.1% of all infections will progress to poliomyelitis, or paralytic polio,3 and only 1 in 1900 poliovirus type 2 infections have such severe consequences even in unvaccinated people.1
Work toward eradicating polio
Progress toward eliminating polio in the Western Hemisphere inspired the World Health Assembly (the World Health Organization’s decision-making body) in 1988 to declare a goal of eradicating polio worldwide by 2000. Live oral polio vaccines (OPVs) were instrumental in the effort to eradicate polio4 as the injectable inactivated vaccine (IPV) prevents poliomyelitis but does not interrupt the chain of transmission of the virus and IPV does not produce mucosal immunity in the gut.1 Unfortunately, while there has been apparent elimination of the wild type 2 strain as a cause of disease, vaccine-derived type 2 poliovirus strains continue to circulate and spread, sometimes in large outbreaks (e.g., 278 cases in Nigeria in 2005 to 2009).4 Only one wildtype strain (type 1) continues to circulate: uninterrupted transmission persists only in parts of Pakistan and Afghanistan. Wild poliovirus cases worldwide have decreased by 99.99% since 1988. Efforts at eradication are ongoing and sustained and increased immunization coverage is needed.5
Because of concerns about rare cases of vaccine-associated paralytic poliomyelitis (VAPP) in OPV recipients and their close contacts (132 cases reported in the U.S. from 1980 to 1995),2 all OPV use in the United States was transitioned to IPV as of the year 2000.1 VAPP is distinct from VDPV: VAPP cases sporadically occur in highly vaccinated communities and do not cause outbreaks, while VDPVs evolve in undervaccinated communities or from prolonged replication in immunocompromised individuals.2
Decreased vaccination rates are cause for concern
Poliomyelitis is almost entirely preventable: three doses of IPV are >99% effective. There are significant concerns that decreased vaccination rates, especially in some communities, will result in more VDPV cases of poliomyelitis in the United States. Only 67% of children <24 months in Rockland County had received three doses of polio vaccine as of July 2020. Perhaps related to the SARS-CoV-2 pandemic, this rate had declined to 60.3% (37.3% in some ZIP codes) as of August 2022.1 Providing some potential reassurance, it is estimated based on data from the CDC’s National Immunization Survey that >95% of children born in 2018 in either Kansas or Missouri have received three doses of polio vaccine, though estimates for the prior few cohorts of children, especially in Missouri, have not been this high6 and subsequent cohorts (no data yet available) may have lower rates as well. Unvaccinated individuals and undervaccinated communities remain at risk for poliomyelitis.
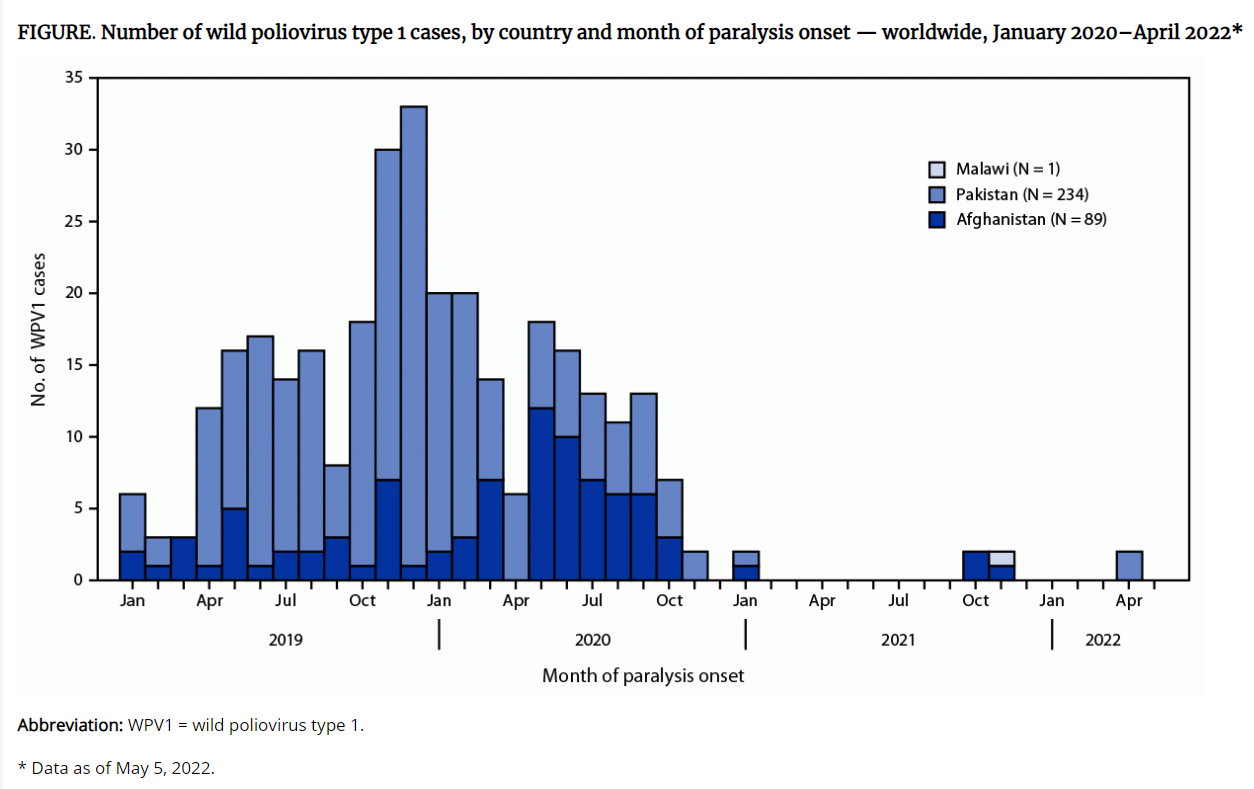
Table source: Reference 5. All material in the MMWR series is in the public domain and may be used and reprinted without special permission.
References:
- Link-Gelles R, Lutterloh E, Schnabel Ruppert P, et al. Public health response to a case of paralytic poliomyelitis in an unvaccinated person and detection of poliovirus in wastewater — New York, June–August 2022. MMWR Morb Mortal Wkly Rep. 2022;71:1065-1068. doi:http://dx.doi.org/10.15585/mmwr.mm7133e2
- Long SS, Prober CG, Fischer M, eds. Principles and Practice of Pediatric Infectious Diseases. 6th ed. Elsevier; 2023.
- Simionescu L, Modlin JF. Poliomyelitis and post-polio syndrome. UpToDate. Accessed September 1, 2022.
- Henderson DA, Klepac P. Lessons from the eradication of smallpox: an interview with D. A. Henderson. Philos Trans R Soc Lond B Biol Sci. 2013;368(1623):20130113. doi:10.1098/rstb.2013.0113
- Rachlin A, Patel JC, Burns CC, et al. Progress toward polio eradication — worldwide, January 2020–April 2022. MMWR Morb Mortal Wkly Rep. 2022;71:650-655. doi:http://dx.doi.org/10.15585/mmwr.mm7119a2
- National Center for Immunization and Respiratory Diseases. (2020, September 28). ChildVaxView. CDC.gov. Accessed September 1, 2022. https://www.cdc.gov/vaccines/imz-managers/coverage/childvaxview/index.html
