While it is understood that diversity and inclusion ultimately benefit everyone, ensuring diversity in research has long presented challenges. Women, ethnic/racial minorities, children, people with disabilities, and those in under-resourced communities who may experience social and educational disadvantages are just a few of the many populations that have been historically underrepresented in research studies. Without including members of diverse populations in research, the results of studies cannot be generalized to historically underrepresented populations, creating a situation that may worsen existing health disparities.
The importance of diversity extends beyond the benefits to underrepresented populations themselves to provide benefit to everyone by ensuring that data and information generated in clinical research studies is accurate. Ensuring representational diversity in clinical trials samples reduces bias in the data generated, leading to more innovative and accurate results and improving the quality of the science. In addition, as datasets are used increasingly to inform healthcare decisions and policy, it is critical that all datasets include all members of the community. With the increasing use of artificial intelligence analytical strategies, unbiased and inclusive data is essential for all to benefit from the inferences drawn from existing datasets.
Including diverse perspectives and voices at the early stages of research projects helps generate ideas and approaches that strengthen the research itself and ultimately benefit everyone involved. In addition, training and mentoring students from diverse backgrounds helps bring new and important ideas and talents into the health field that will increase the impact of research.
An Unwavering Commitment to Research that Helps Everyone
As the Children’s Mercy Research Institute (CMRI) advances its mission of accelerating transdisciplinary research to improve the health and well-being of children, it continues to explore innovative ways to bolster diversity and inclusion and foster engagement within the CMRI and with research participants, families and community partners.
This commitment to enhanced engagement aims to ensure that research projects, Hospital services, research participants and even the words we use when discussing race and ethnicity appropriately reflect the diversity of the patients and families served by Children’s Mercy.
“Diversity in pediatric research means ensuring all children and families regardless of race, ethnicity, language, economic status, education level, ability, gender identity, or sexual orientation have an opportunity to participate in research,” says Andrea Bradley Ewing, who serves as the Director of Community Engaged Research at Children’s Mercy. “This means ensuring communities that have historically been harmed by research or underrepresented in research are adequately represented in all research so the scientific community is more aware of effective interventions and treatments that benefit all children.”
Diversity and Inclusion Part of CMRI’s DNA
CMRI incorporates diversity and inclusion into its overall strategic plan to ensure that all patients, families, and communities benefit from the scientific breakthroughs that advance treatment and improve care. Some of these efforts include:
- Exploring innovative and effective measures to integrate diversity throughout research through work conducted by the Inclusion and Diversity in Research Work Group
- Ensuring all facets of work include diversity and inclusion to train the next generation of researchers and scientists (as in the STAR 2.0 program)
- Engaging diverse community voices through the CMRI Community Advisory Board on the best ways to develop, implement and disseminate research
- Recruiting faculty and research coordinator/research assistant candidates from underrepresented communities
- Recruiting and retaining bilingual research staff who are focused on ensuring non-English speaking patients and families are not excluded from research based solely on language
- Providing resources for research teams that engage diverse research participants in their projects, like the translation of study documents provided by the Office of Research Integrity
- Developing mechanisms and tools to enable research teams to track and report their inclusion of diverse races, ethnicities and genders in their research projects
CMRI’s commitment not only involves efforts to recruit and retain diverse research participants but to also prioritize diversity and inclusion when it comes to implementing studies that enhance community engagement; promoting research that addresses health disparities; and supporting work with businesses that advance diversity, equity and inclusion practices in the communities we serve.
Diversity in pediatric research means ensuring all children and families regardless of race, ethnicity, language, economic status, education level, ability, gender identity, or sexual orientation have an opportunity to participate in research.
In addition, CMRI’s efforts reflect recent guidance from the American Academy of Pediatrics and the Journal of the American Medical Association on the use of race, ethnicity, and inclusive language. To promote a culture that values inclusion, equity, and diversity, CMRI leadership are committed to using language that is free from bias and affirms all races, ethnicities, genders, abilities, and sexual identities.
Community-based studies center on needs of Hispanic and LatinX communities
Several current research studies at CMRI aim to directly impact the health and well-being of those in the Hispanic and LatinX communities.
Jordan Carlson, PhD, and his team are participating in the Hispanic Community Health Study/Study of Latinos (HCHS/SOL), a national study exploring the role of acculturation in the prevalence and development of disease. The multicenter study is also working to identify those factors playing a role in the health of those in the Hispanic and LatinX communities.
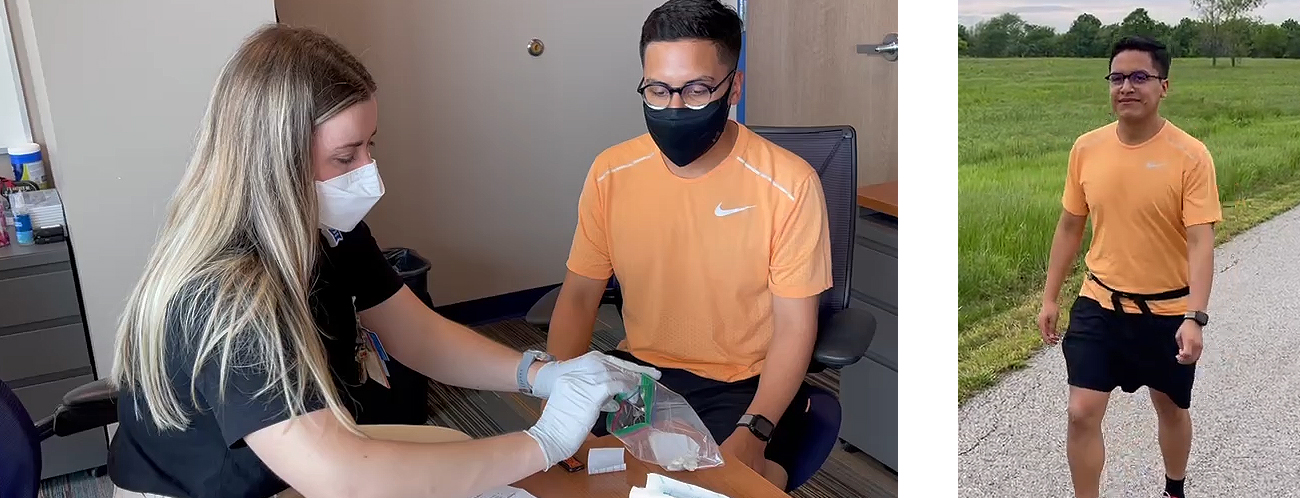
Dr. Carlson and his team are working on two projects in the national study – called SOL VIDA and SOL CASAS – that, respectively, investigate the link between sedentary patterns and cardiovascular disease, and test a model of neighborhood environment factors, physical activity, and psychosocial issues like depression and stress on changes in cardiometabolic health in Hispanics/Latinos.
On a more local level, Dr. Carlson leads two community-based studies that focus on structurally disadvantaged communities in the Kansas City area. A project with Our Healthy Jackson County aims to provide residents with tools and support to bolster their levels of physical activity.
“By focusing on diverse perspectives and communities in this research, the outcomes are more likely to lead to improvements in community health that benefit all residents of Kansas City,” says Dr. Carlson.
In addition, through an award funded by the National Institutes of Health and the Environmental Protection Agency, Dr. Carlson and Dr. Jannette Berkley-Patton (UMKC) and their teams are collaborating with the University of Missouri – Kansas City, University Health, BikeWalkKC, Kansas City Public Works, and the Kansas City Area Transportation Authority to study a new policy that eliminated bus fare citywide in Kansas City. The team is evaluating the policy’s impact on health factors such as physical activity, healthy eating, weight status, and economic barriers to health in order to determine whether the policy could be continued and expanded in other cities across the US as a way to support health in structurally disadvantaged communities.
Everyone benefits when community environments are designed to support health, and efforts to improve community environments are more likely to be successful when they are inclusive.
Another research project, funded by the Katharine Berry Richardson Foundation and led by Ayanda Chakawa, PhD, is exploring the disparities in seeking help and navigating care access pathways for pediatric behavioral health for youth from Black, Indigenous, and People of Color (BIPOC) groups and socioeconomically disadvantaged backgrounds. The one-year pilot project aims to develop culturally informed pathways that can facilitate families’ care navigation access to behavioral health services for their children. Data collection and care navigation intervention will be provided with English and Spanish language options to account for the majority languages represented among the target sample. Using a community engaged research approach, Dr. Chakawa’s project involves partnership with the Children’s Mercy “El Consejo de Familias Latinas/Hispanas” and “Mental Health” Patient Family Advisory Councils (PFACs) to help maximize the impact of the research based on these PFACs diversity, equity, and inclusion perspectives and as experts on the needs of children served through Children’s Mercy and challenges faced in accessing needed care.
“Though my study specifically focuses on working to understand disparities in care among BIPOC populations, all patients served through the PCC within the target study age range have the opportunity to participate in the study as the goal is to provide equitable access to care across all groups served,” says Dr. Chakawa.
Fortifying relationships, building trust in the clinic and in research

To further support the needs of those in the Hispanic and LatinX communities, Children’s Mercy has three different clinics dedicated to serving Spanish-speaking families – the Spanish Oncology Clinic, Spanish Epilepsy Clinic and the CHiCoS Clinic. The trusting relationships Children’s Mercy bilingual staff build with these patients and families and the unique focus on their cultural and genetic differences can make a substantial difference in their treatment and outcomes.
Terrie Flatt, DO, Director of the Program for Clinical Oncology Services and Research for Hispanics, established the Spanish Oncology Clinic at Children’s Mercy in 2012 to address genetic differences in the Hispanic population, which has the highest incidence of acute lymphoblastic leukemia and the worst outcomes. While the clinic initially focused on language, Dr. Flatt noted that the focus quickly shifted to the differences in the population related to genetics, disease responses, medication tolerance and toxicity with certain chemotherapies.

Launched in 2017 by Lines Vargas Collado, MD, the Spanish Epilepsy Clinic aims to improve treatment through building trust and understanding the cultural context for any misconceptions in the Hispanic culture about epilepsy. The condition may be seen as a social barrier and assumptions persist about the ability of a person who has epilepsy to have a family or maintain a job. Patients who have epilepsy may experience a stigma and, as a result, feel socially isolated and avoid medical care. Addressing families in a culturally sensitive manner, providing education and communicating in their language help with treatment compliance.
Clínica Hispana de Cuidados de Salud (CHiCoS) translated is the Spanish Health Care Clinic – and it is a Lifeline for Spanish-speaking parents looking for care in Kansas City. Established in 2008 by John (JC) Cowden, MD, MPH, and now under the direction of Jodi Dickmeyer, MD, the CHiCoS Clinic serves the primary care needs of the Spanish-speaking community through providers who are linguistically and culturally competent to care for them. The clinic also trains bilingual residents through the Culture and Language Coaching Program at Children’s Mercy, which aims to professionalize the use of Spanish in the health care and social service settings.

The commitment to having bilingual staff available to help build relationships with Hispanic and LatinX communities extends to research as well and the growing number of personnel who earn Qualified Bilingual Staff (QBS) certification.
“Having QBS-certified research personnel is crucial to carry out inclusive projects that will benefit all children,” says Susana Chavez-Bueno, MD, of the Division of Infectious Diseases. “Patients and families need to clearly understand in their own language what a research project is about before deciding to participate. QBS-certified staff facilitate increased representation of children who would otherwise be excluded from participating in research due to language barriers. Their work is essential to obtaining reliable research results that are applicable to broader pediatric populations.”
When we root research and clinical work in diversity, equity, and inclusion (DEI) efforts, it doesn’t only highlight the needs of those from minoritized or historically disenfranchised groups. It serves as a benefit to all groups because it necessitates developing and implementing efficient and tailored strategies that result in best care for everyone. This can lead to extremely beneficial changes on multiple levels for how medical facilities offer pediatric healthcare for all people.
CMRI recognizes that supporting projects such as these and fostering a diverse and inclusive workforce will not only strengthen trust in the community the institution serves, but it will also advance science and promote the health and wellbeing of children everywhere. “When we root research and clinical work in diversity, equity, and inclusion (DEI) efforts, it doesn’t only highlight the needs of those from minoritized or historically disenfranchised groups. It serves as a benefit to all groups because it necessitates developing and implementing efficient and tailored strategies that result in best care for everyone. This can lead to extremely beneficial changes on multiple levels for how medical facilities offer pediatric healthcare for all people,” adds Dr. Chakawa.