Visual Diagnosis: A Scaly Truncal Eruption
An 11-year-old boy presents with a four-week history of a mildly pruritic rash on the trunk. He has a history of nummular dermatitis, which had significantly improved with topical steroids and regular emollient use.
Approximately four weeks prior to presentation, his parents noticed a scaly patch on the chest. Over the following one to two weeks, additional similar lesions developed and spread across the chest and back. The rash has been mildly itchy but not painful, and it has not interfered with sleep or daily activities. There have been no associated systemic symptoms, including fever, sore throat, cough or malaise. He has not had any recent medication changes, new personal care products or known exposures. No one else at home has a similar rash.
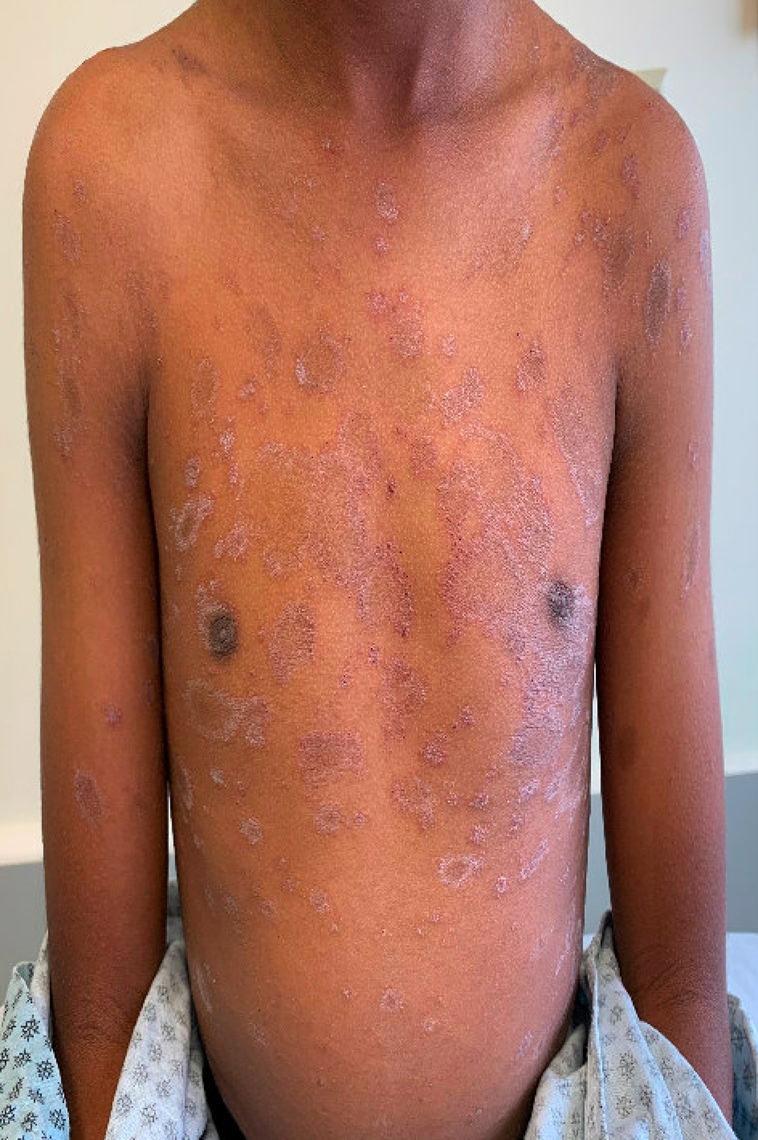
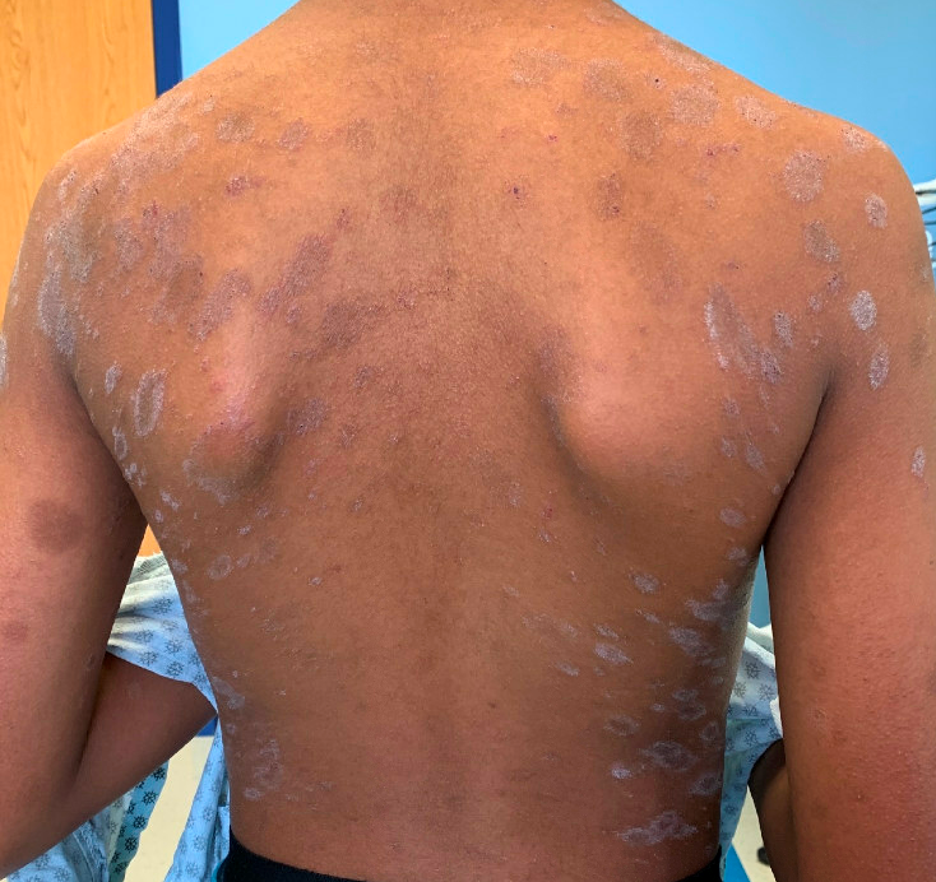
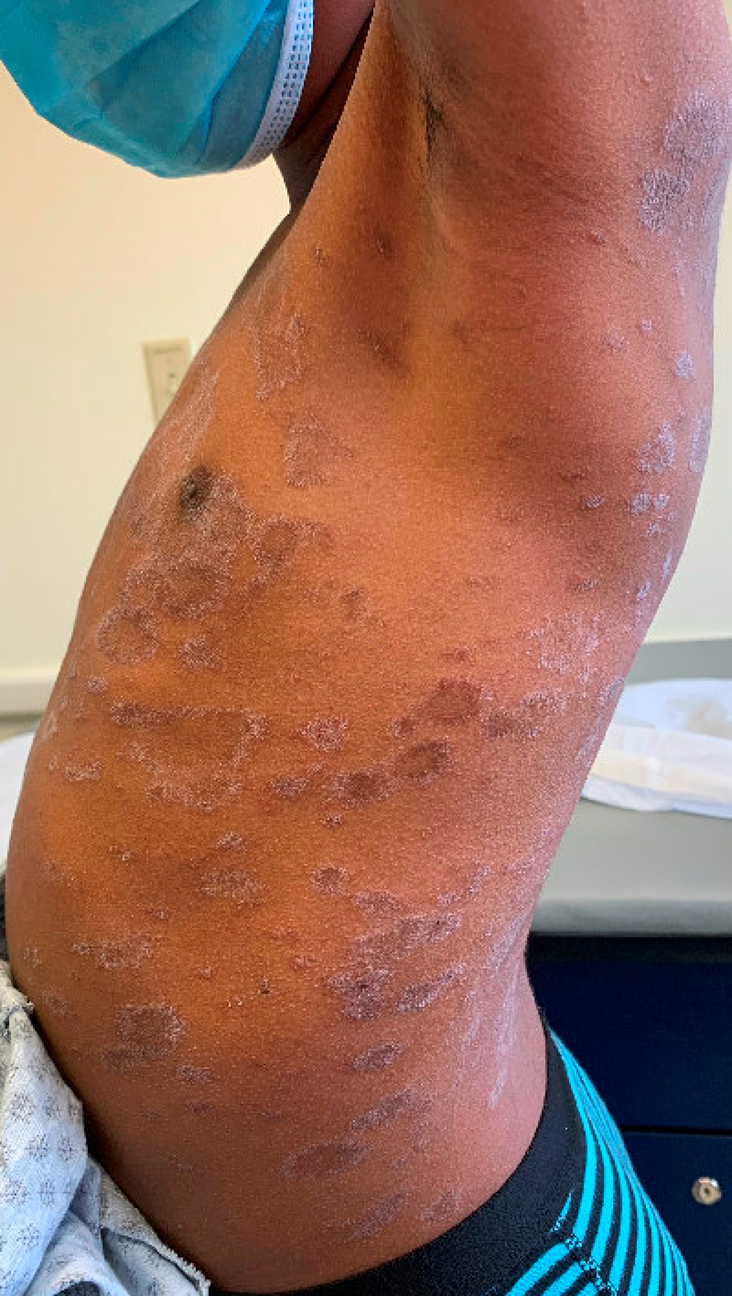
Question 1: What is the most likely diagnosis?
A. Pityriasis rosea
B. Tinea versicolor
C. Pityriasis lichenoides chronica
D. Psoriasis
E. Nummular dermatitis
Correct Answer: A. Pityriasis rosea
Explanation:
This patient’s eruption is most consistent with pityriasis rosea based on the morphology, distribution and clinical course. The history of an initial solitary scaly lesion on the chest, likely representing a herald patch, followed by a generalized eruption over the trunk is a classic presentation. On examination, the presence of oval plaques with fine peripheral scale oriented along relaxed skin tension lines produces the characteristic “Christmas tree” pattern that is highly suggestive of this diagnosis.
In children with darker skin types, pityriasis rosea can appear more hyperpigmented or violaceous rather than erythematous. While the patient presented with more typical pityriasis rosea, another variant where lesions may be more papular than plaque-like, referred to as “papular pityriasis rosea,” is seen more commonly in patients with skin of color. This can make recognition more challenging and increases the likelihood of misdiagnosis.
- Tinea versicolor can present with scaly patches or thin plaques and may be hyperpigmented, hypopigmented or pink, particularly in patients with skin of color. However, the scale in tinea versicolor is typically more diffuse and powdery rather than forming a collarette at the periphery of lesions. The distribution also differs, as tinea versicolor favors the upper trunk, neck and proximal arms and does not follow relaxed skin tension lines or produce a “Christmas tree” pattern. In addition, there is no herald patch. A negative KOH preparation further argues against this diagnosis.
- Pityriasis lichenoides chronica (PLC) presents with crops of small, red-brown papules that may develop a fine scale, but the scale is typically subtle and not characterized by the peripheral collarette seen in pityriasis rosea. PLC often involves the trunk and proximal extremities and can have a somewhat symmetric distribution, which is why it is frequently confused with pityriasis rosea. However, the distinction lies in the lesion morphology and clinical course. Lesions in PLC tend to be smaller and more monomorphic, and appear in multiple crops at different stages of evolution, often persisting or recurring over weeks to months.
- Psoriasis generally produces thicker, well-demarcated plaques with more prominent, diffuse scale. Pediatric psoriasis often involves the scalp, extensor surfaces or intertriginous areas and may be associated with nail changes or a family history. The lesions in this case are thinner, more oval, and distributed in a pattern that is not typical for psoriasis.
- Nummular dermatitis presents with coin-shaped eczematous plaques that are often more exudative, crusted and intensely pruritic. While this patient has a prior history of nummular dermatitis, the current eruption differs in morphology, distribution and symptoms, and does not resemble his prior flares.
Pediatricians should also be aware of clinical variants of pityriasis rosea. Papular pityriasis rosea, which is more common in children and patients with darker skin, may lack the classic plaque morphology, instead presenting with small scaly papules that also follow relaxed skin tension lines. Inverse pityriasis rosea presents with scaly plaques in the axillae, neck or groin rather than the trunk. Recognition of these variants is important to avoid unnecessary antifungal or antibiotic treatment.
Question 2: What is the most likely underlying etiology of this condition?
A. Dermatophyte infection
B. Reactivation of human herpesvirus 6 or 7
C. Autoimmune T-cell–mediated disease
D. Bacterial toxin-mediated process
E. Malassezia overgrowth
Correct Answer: B. Reactivation of human herpesvirus 6 or 7
Explanation:
Although the exact cause of pityriasis rosea is not definitively established, the leading hypothesis is that it represents a viral exanthem related to reactivation of human herpesvirus 6 or human herpesvirus 7. Multiple studies have demonstrated the presence of viral DNA in lesional skin and peripheral blood, supporting this theory.
This viral association helps explain several clinical features of pityriasis rosea, including its self-limited course, occasional mild prodromal symptoms, and seasonal clustering. Importantly, despite this presumed viral trigger, pityriasis rosea is not considered contagious, and children can continue normal school and social activities.
The other answer choices reflect conditions that may be considered in the differential diagnosis but do not explain the overall clinical picture. Dermatophyte infection and Malassezia overgrowth would be expected to produce positive findings on KOH examination, while autoimmune and toxin-mediated processes do not align with the characteristic morphology and natural history of this eruption.
Question 3: Which of the following statements regarding treatment is most accurate?
A. Oral antifungals are first-line therapy.
B. High-potency topical steroids shorten disease duration.
C. Oral acyclovir may shorten the course in some patients.
D. Antibiotics are recommended to prevent secondary infection.
E. Phototherapy is contraindicated.
Correct Answer: C. Oral acyclovir may shorten the course in some patients.
Explanation:
Pityriasis rosea is a benign, self-limited condition that typically resolves within two to three months without treatment. Management is therefore primarily focused on patient and family reassurance and symptomatic relief of pruritus.
Several small studies have suggested that oral acyclovir, particularly when initiated early in the course of the disease, may shorten the duration and reduce the severity of the eruption. However, because pityriasis rosea resolves spontaneously, antiviral therapy is not routinely required and is generally reserved for patients with more severe or extensive disease.
Topical corticosteroids and oral antihistamines can be helpful for managing itch but do not alter the natural history of the condition. Antifungal therapies are not effective, as this is not a fungal infection, and antibiotics have no role in treatment. Phototherapy, particularly narrowband UVB, may be considered in selected cases and is not contraindicated.
For pediatricians, one of the most important aspects of management is avoiding unnecessary treatments and investigations. A negative KOH preparation and a classic clinical presentation can help prevent prolonged courses of antifungals or antibiotics, which are commonly prescribed when the diagnosis is uncertain.
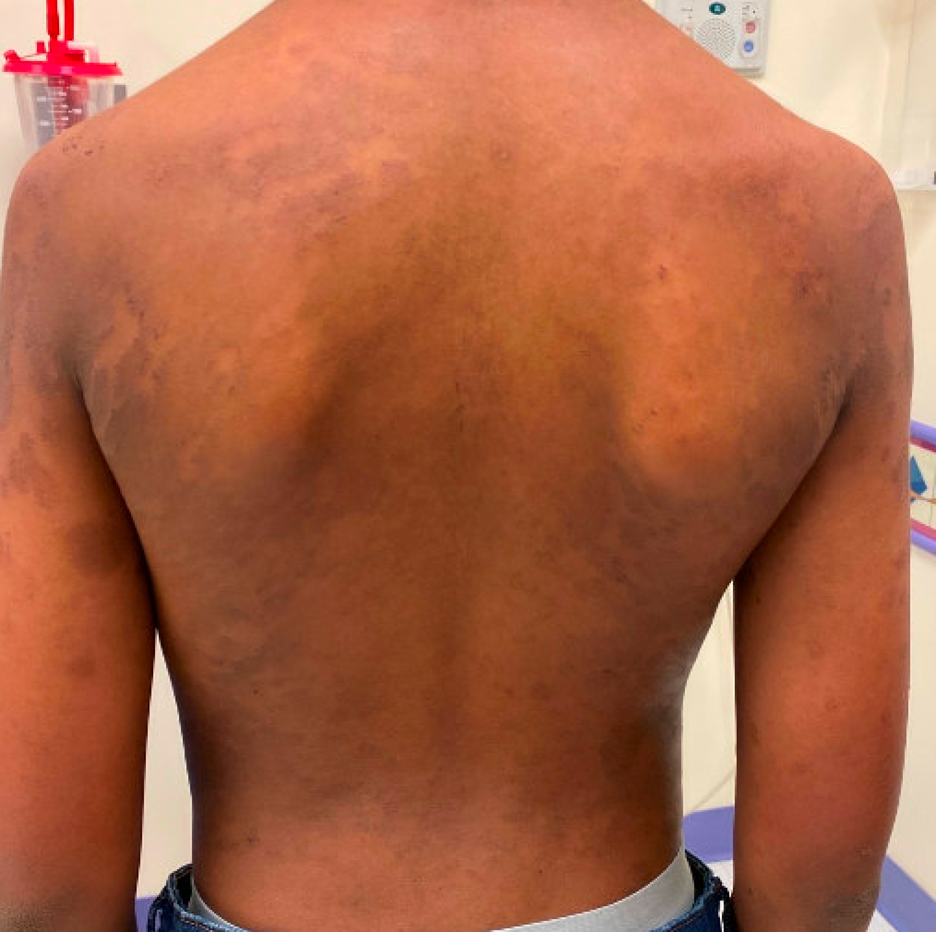
Bottom Line for Pediatricians
Pityriasis rosea should be suspected in children who present with an initial herald patch followed by a generalized eruption of oval, scaly lesions distributed along skin tension lines. Recognition can be more challenging in patients with darker skin, where lesions may appear hyperpigmented or papular rather than as erythematous plaques. The condition is self-limited and non-contagious, and most often requires only reassurance and symptomatic treatment, with antiviral therapy reserved for select cases.
The patient was seen for follow-up a month after his initial visit with significant improvement in the eruption with some residual post inflammatory dyspigmentation.
References:
- Leung AKC, Lam JM, Leong KF, Hon KL. Pityriasis rosea: an updated review. Curr Pediatr Rev. 2021;17(3):201-211. doi:10.2174/1573396316666200923161330
- Villalon-Gomez JM. Pityriasis rosea: diagnosis and treatment. Am Fam Physician. 2018;97(1):38-44. https://www.aafp.org/pubs/afp/issues/2018/0101/p38.html
- Urbina F, Das A, Sudy E. Clinical variants of pityriasis rosea. World J Clin Cases. 2017;5(6):203-211. doi:10.12998/wjcc.v5.i6.203
Associate Program Director, Pediatric Dermatology Fellowship; Assistant Professor of Pediatrics, University of Missouri-Kansas City School of Medicine; Clinical Assistant Professor of Internal Medicine, University of Kansas School of Medicine