Clinical Experience
Pediatric Surgery Fellowship
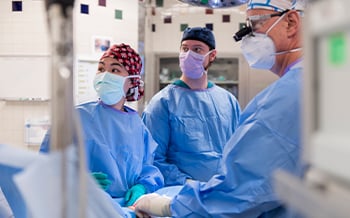
Goals of the Pediatric Surgery Fellowship are accomplished by:
-
Fellow participation in and supervision of the pediatric surgical service under faculty direction.
-
Fellow participation in and supervision of pediatric surgical critical care patients under faculty direction.
-
Fellow participation in outpatient evaluation and management of common conditions referred to pediatric surgeons as well as preoperative and post-operative evaluation of patients seen in consultation.
-
Operative experience emphasizing all areas of pediatric general and thoracic surgery, including surgical endoscopy and minimally invasive procedures.
It is assumed that the fellow has developed basic skills as a general surgeon and that he/she is capable of organizing a surgical service from a fellow’s perspective. Over the course of two years, the fellow will be allowed graduated responsibility for formulating the differential diagnosis for a patient’s symptoms, for developing a plan of treatment, and for implementing the treatment plan. One fellow will always be senior to the other two and will serve as an educational resource to the other PSFs, but the primary responsibility for the education of the pediatric surgical fellow lies with the attending staff. The fellow is “on call” with and supervised by one of the staff surgeons.
During the two years of training, the PSF will encounter a broad exposure to general, thoracic, urologic, and minimally invasive surgery. During the first year, one month is often spent in the Neonatal Intensive Care Unit. Goals and objectives of this rotation include a thorough understanding of the nutritional requirements, ventilatory management, and management of the infant on ECMO as well as an exposure to the general pathophysiology of newborns. As the fellow progresses through this two-year period, he/she will be expected to make the transition from a novice in the area of pediatric surgery to being capable of practicing pediatric surgery independently and confidently in either an academic or private setting.
Rounds on the pediatric surgical service begin at 6:00 a.m. to allow complete evaluation of all the patients on all of the units prior to the day’s operating schedule. Early electronic order entry and progress notes for the day establish appropriate communication and clinical plan development with both the nursing staff as well as with other consulting services. These activities should be accomplished prior to either conferences or the start of scheduled operations during the day. The completion of the progress notes involves a team effort for the PSFs, the rotating junior general surgical residents, and the nurse practitioners. These notes and orders are entered electronically. The PSFs are responsible for assigning the work on rounds, as well as ensuring completion of the work throughout the day, and final review on evening rounds. The Chief PSF is expected to have assigned individual operative cases to all the fellows/residents. History and physicals as well as consent forms must be completed in order to allow for efficient progress of care.
Within the course of the operation, the PSF is responsible for understanding the operation and having reviewed the indications for and basic techniques of any new procedure, or any procedure that is begun with an attending whom they have not operated with before. This allows for efficient discussion of the operative case, patient safety, and expeditious operative management. The PSF is responsible for writing post-operative orders on all patients, home discharge orders, and home care for those patients whom he or she is managing directly. If the patient is transferred to the NICU or PICU, the PSF is responsible for writing all post-operative orders and for arranging appropriate communication with the nursing staff in order to maintain post-operative care of that patient throughout the course of the patient’s stay in the unit. The pediatric surgery service will assume primary care of those patients unless otherwise specified. A clear short- and long-term care plan must be understood. For that reason, the PSF must establish appropriate lines of communication between the general surgery residents and the attending staff. Any changes in the patient’s condition must be communicated directly to the responsible attending or the covering attending in order to review the care plan and take the appropriate action.
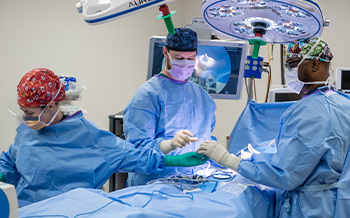
Outpatient Management
The PSFs will attend at least weekly outpatient clinics to gain exposure to diverse outpatient management of pediatric surgical patients.
Quality Improvement
The fellows participate in interdisciplinary clinical quality improvement and patient safety programs. This is accomplished through a monthly lecture series for fellows in the hospital. The fellows and faculty must demonstrate an understanding and acceptance of their role in the assurance of the safety and welfare of patients for whom they are providing care, the provision of patient and family-centered care, an assurance for fitness for duty, efficient management of their time before, during, and after clinical assignments, recognition of impairment, including illness and fatigue in themselves and also in their fellow residents and staff, an attention to lifelong learning, and an honest and accurate reporting of duty hours, patient outcomes, and clinical experience data. Also, the faculty will monitor the fellow’s patient care performance improvement indicators.
Case Load
Because of an extensive operative case-load, the PSFs reach the completion of their two years in the training program with an operative experience which allows them to transition into a staff position with a great deal of confidence in their own judgment and technical abilities.
Our Pediatric Surgery Fellowship team
Rebecca Rentea, MD
Program Director
(816) 234-3575
rrentea@cmh.edu
Danelle Vogt, MBA
Program Coordinator
(816) 983-6875
dkvogt@cmh.edu