Myocarditis: Callan’s story

Callan’s parents, Jill and Clint, knew something was wrong. Callan — a 5-year-old cowboy with an old soul — had been treated for influenza and a double ear infection at their local clinic this winter, but he just wasn’t getting better. Now this kind and patient kid’s hands and feet were ice cold, his color had gone white, and he was throwing up what looked like coffee grounds.
“I was worried about internal bleeding,” said Jill, who works as a medical coder. “God was telling me, ‘You need to get this kid somewhere now.’” She and Clint took Callan to their emergency room in Sabetha, Kan., where they asked for a CT scan. His white blood count was off the charts, and the CT showed an inflamed gallbladder. Children’s Mercy sent their Critical Care Transport jet to bring Callan to our Adele Hall Campus.
His flu symptoms were being monitored when Callan’s heart stopped. His parents and pastor were at his side. “Callan loves the Lord, his family, tractors, monster trucks and all animals,” said Jill. And, suddenly, they were losing him.
A plan for the unthinkable
Fortunately, Children’s Mercy has a detailed plan for how to handle cardiac arrests outside of our intensive care units (ICUs). “We knew our process, and our team was ready,” said Jenna Miller, MD, pediatric intensivist and Pediatric ECMO Director, Critical Care Medicine.
The first two responders to Callan’s room were Mackenzie Johnson, BSN, RN, CCRN, PICU Assistant Director of Nursing, and Michelle Brown, DO, pediatric intensivist, Critical Care Medicine.
Jill calls them “two angels here on earth.” They were part of a very large multidisciplinary team who supported this remarkable kid through an unimaginable ordeal with myocarditis.
Dr. Brown started chest compressions and activated extracorporeal cardiopulmonary resuscitation (ECPR): A multidisciplinary team needed to perform CPR on Callan while traveling down several floors to the PICU where Callan could be put on extracorporeal membrane oxygenation (ECMO). ECMO would act as Callan’s heart and lungs to keep him alive.
“[ECPR] is extremely time-sensitive,” said Dr. Miller. “Everyone has to be operating at a high level, including the bedside staff, surgeons and the ECMO team.”
“The outcomes are measured in minutes,” said Andrew Ausmus, MD, cardiac pediatric intensivist, Critical Care Medicine. “A difference of five minutes makes a measurable difference in the chance a patient is going to survive.”
A concerted team effort
“Seeing our ICU nurses jump into action was incredible,” said Dr. Brown. “There is a sense of communication without even having to use a word. When Mackenzie ran into the room, she met my eyes and said, ‘I’ll take over chest compression so you can continue to run the code.’”
The 10-person resuscitation team traveled with Callan to the elevator, down to the PICU, and into the only open room in the very busy unit to join the ECMO team. They had around 15 team members inside the room and more outside.
“It’s a very coordinated, orchestrated kind of movement,” said Niranjan Vijayakumar, MBBS, cardiac pediatric intensivist, Critical Care Medicine.
While surgeons were working to get Callan on ECMO, the team noticed there was fluid collecting outside his heart, compressing it and making it difficult for blood to flow through the machine. Steve Kaine, MD, FAAP, FACC, FSCAI, pediatric cardiologist, was walking by and immediately scrubbed to perform an emergent pericardiocentesis to drain that fluid.
Callan also had critically high potassium levels (hyperkalemia), so the Nephrology team put him on emergent dialysis as well.
One surprise after another
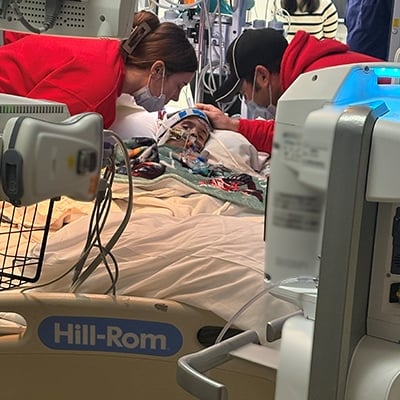
Once Callan was on life support, his family joined him in the PICU. They tried to hold him around all the lines and medical equipment.
“We found out later that he was [on CPR] for 41 minutes,” said Jill. “Just seeing him cold and lifeless — it’s hard to wrap your brain around that. Even though it’s hard, God still met us where he needed to. He aligned that rapid response team to be there for Callan at the right time.”
Callan’s heart wasn’t showing any signs of pulsatility: his heart wasn’t contracting or sending any blood to his body on its own. The team believed he would need a heart transplant to survive. But Callan wasn’t done surprising everyone.
Toby Rockefeller, MD, Medical Director, Interventional Cardiology, performed a left atrial vent to drain and depressurize Callan's heart. Afterward, they started seeing electrical activity return and signs that his heart was starting to contract again — unusual after so long without activity.
“It was just days of praying over him and talking to him and hoping for the best,” said Jill. “Now he was starting to move his fingers, his hands and open his mouth.”
But there was a new concern: Callan had a high level of blood clots in the left side of his heart. If those clots dislodged with his strengthening heart activity, they could go straight to the brain.
“There was a lot of worry and discussion about how to decrease the risk of [stroke],” said Dr. Ausmus. With careful monitoring and anticoagulants, the clots dissolved on their own — another very rare occurrence.
As Callan regained heart function, his team concentrated on his lungs. They scanned them for damage and did a bronchoscopy to get Callan ready to breathe on his own again.
Callan’s heart and lungs were strong enough to get off ECMO after 12 days. He continued dialysis but was able to stop much earlier than expected, shortly after transferring out of the CICU.
It’s the people
Callan’s heart arrhythmias are now medically managed. He’s been working with Occupational Therapy, Physical Therapy and Speech Therapy and making quick progress — walking unassisted and throwing spirals with his football! To his mom’s chagrin, he’s also starting to quote some of The Sandlot’s saltier lines when he gets impatient with his PTs and OTs. He was released from the hospital 43 days after he first arrived.
Callan’s neuro MRI shows a few stroke-like changes on the right side of his brain, but his chances at a full recovery are high — such a positive neuro-outcome after 41 minutes on CPR is extremely uncommon.
“He’s recovering both spirits and strength with every passing day,” said Dr. Vijayakumar, who said Callan’s post-hospital goal is to go to a monster truck rally as soon as possible.
Callan has had a rally of his own during his recovery.
“There were people all over the world praying for Callan,” said Jill. “Science and faith are a dream team — miracles and medicine.”
An incredible family, a phenomenal team

Callan’s care team has been reflecting on his against-all-odds medical events and the careful preparation that helped them serve him well.
“This was one of the best collaborative, multidisciplinary cases I have ever seen,” said Dr. Miller. “Perseverance and willingness to continue conversations, think outside the box and give him every chance possible is what led to this outcome.”
Another key factor? The close ties between the PICU and CICU. “The fact that we’re right next to each other and able to collaborate makes a case like this a little bit easier,” said Dr. Ausmus.
Dr. Brown said Callan’s family was an important part of the team. “On a day they would consider a living nightmare, they were tuned in, asked insightful questions and were heavily engaged in his care all along the way,” said Dr. Brown.
The respect is mutual. “We truly believe the doctors, nurses, and staff at Children’s Mercy are the hands and feet of Christ here on earth,” Jill wrote in an update to their friends and family. “From physicians and nurses, to security, front desk staff, Palliative Care, Child Life, all the people behind the scenes we haven't even met, Environmental Services and the Ronald McDonald House rooms and homes — every single person has reflected God’s love.”
Dr. Brown echoed that gratitude for her Children’s Mercy team members.
“It’s the people, hands down,” said Dr. Brown. “It’s pretty phenomenal to be part of a team like this.”
